Testing for Diabetes in Children

Diabetes mellitus can be a devastating illness, especially when it comes on suddenly in a child or adolescent. In young people it is usually so-called Type 1, or insulin-dependent diabetes, an autoimmune disease in which the immune system attacks the insulin-producing beta cells in the pancreas. The disease can have a major impact on the whole family, and sometimes people forget the way in which it can affect siblings whose needs often need to be subordinated to the needs of the newly diagnosed young person.
And here is an important point: even when it appears suddenly, the disease process may have been going on for some time before the clinical symptoms appear. By the time that blood glucose levels begin to rise, it usually implies that the damage to the insulin-producing cells in the pancreas has reached a critical point, and the chance of recovery is low. Anything that we can do to prevent the disease from progressing to the point of producing symptoms would be immensely helpful, and that starts with early recognition before the pancreatic damage has reached critical.
Although we now understand a great deal about the interplay of genetic, environmental and immunological factors that may lead to the illness, this knowledge has so far not helped us very much. There has been a tremendous need to try and identify the early stages of the disease, but that goal has been elusive.
In a study published in the Journal of Immunology researchers from the University of Queensland’s Diamantina Institute for Cancer, Immunology and Metabolic Medicine, are developing a simple test that may predict whether a child will develop Type 1 diabetes. They have identified a cellular pathway known as NF-kappa B that is activated in certain blood cells – monocytes and dendritic cells – of people with Type 1 diabetes.
In healthy people monocytes remain quiescent unless they are activated by an infection or other stressor. Then the NF-kappa B pathway gets activated.
In people with Type 1 diabetes things work the other way round: monocyte NF-kappa B was already activated in the blood, and when exposed to infection the pathway shut down. This tells us that there is a problem of immune control that may cause diabetes to develop in children. It is this monocyte abnormality that will hopefully form the basis of a diagnostic test.
This work is assuming more urgency since there are several trials of diabetes vaccines underway, and if successful, it may become possible to identify and intervene in children at risk of Type 1 diabetes before it occurs.
In addition, understanding why the immune system loses control before the disease starts should open up a number of new options for prevention and treatment.
A Virus Linking Depression, Aging and Heart Disease

We have known for a long time that there are close links between depression, aging and heart disease, but the nature of the link has remained elusive. Most of the smart money has been on inflammation, but there could be other candidates.
New research in the journal Brain, Behavior and Immunity has linked an increase in two inflammatory proteins in the immune system with a latent viral infection and proposes a chain of events that might accelerate cardiovascular disease. It is possible that the same process may be involved in a number of other ailments that can afflict us, as we get older. The findings also suggest that chronic depression may play a key role in initiating the cascade that can lead to the development of coronary artery disease.
It has been known for some time that increased levels of the proinflammatory cytokines, TNF-α and IL-6, predict mortality and morbidity. High levels of each of them are found in the plasma and in atherosclerotic lesions of people with cardiovascular disease.
The levels of IL-6 in the body increase as the immune system ages. Some of the IL-6 is generated by immune cells – macrophages – that go to the site of an infection or injury. Earlier work by the team also showed that increases in psychological stress and depression could substantially raise the levels of IL-6 and TNF-α in the body.
Increased stress and depression can also trigger latent viruses to reactivate and begin reproducing inside cells. The viruses of greatest interest are some herpes viruses such as the Epstein-Barr virus (EBV). We know that up to 90% of the people in North America have been infected by EBV by the time they are adults.
If EBV begins to multiply in cells in the body, it produces a protein called dUTpase that, in turn, can stimulate macrophages to make yet more IL-6.
The researchers developed a model to test these linkages by using endothelial cells that line the inside of veins in umbilical cord tissue. I spent years working with these cells myself, and they provide an excellent substrate for examining vascular responses and the interaction between blood vessels and macrophages when exposed to the virus as well as the dUTpase protein.
As expected, the production of IL-6, as well as TNF-a, were increased just as they would be as part of the inflammatory process in the body. Such chronic incidents of inflammation are integral to the onset of atherosclerosis and an array of other diseases.
This work suggests a new way of thinking about how vascular diseases develop. We carry around these latent herpes viruses in our bodies virtually all our lives and periodically they can hurt us as we age, develop depression or, perhaps a nutritional imbalance.
Taken together with the recent data on the physical effects of loneliness, if you want to live a long and healthy life:
- Watch you mood: depression can kill you
- Stay socially engaged: loneliness can be fatal
- Maintain a balanced diet
- Take some physical exercise every day
- Learn – and practice! – some simple stress management techniques. You can obtain some at RichardGPettyMD.com
Molecules of Loneliness

It is well known that our social environment has a major impact on our health, wellness and longevity. Lonely, socially isolated adults have a higher mortality than those who are socially engaged.
There has been a lot of speculation about the factors involved, and there is a fascinating study published in the current issue of the journal Genome Biology.
Researchers from UCLA identified a distinct pattern of gene expression in the white blood cells of people who experience chronically high levels of loneliness. The findings suggest that feelings of social isolation are linked to alterations in the activity of some of the genes that drive inflammation providing a molecular framework for understanding why social factors are linked to an increased risk of heart disease, viral infections and cancer.
Lonely people suffer from higher mortality than people who are not, and the debate has been whether that risk is a result of reduced social resources, or whether it is biological.
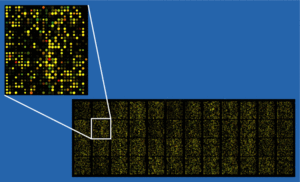
In this study the researchers used DNA microarrays to survey the activity of all known human genes in white blood cells from 14 individuals in the Chicago Health, Aging, and Social Relations Study. Six participants scored in the top 15% of the UCLA Loneliness Scale, a widely used measure of loneliness that was developed in the 1970s; the others scored in the bottom 15%. The researchers found 209 gene transcripts that were differentially expressed between the two groups, with 78 being over-expressed and 131 under-expressed. Genes over-expressed in lonely individuals included many involved in immune system activation and inflammation. At the same time, several other key gene sets were under-expressed, including those involved in antiviral responses and antibody production.
The first author on the study s Steve Cole, an associate professor of medicine in the division of Hematology-Oncology at the David Geffen School of Medicine, and a member of the UCLA Cousins Center for Psychoneuroimmunology, and he had this to say:
“What this study shows is that the biological impact of social isolation reaches down into some of our most basic internal processes the activity of our genes.
We found that changes in immune cell gene expression were specifically linked to the subjective experience of social distance. The differences we observed were independent of other known risk factors, such as health status, age, weight, and medication use. The changes were even independent of the objective size of a person’s social network.”“We found that what counts at the level of gene expression is not how many people you know, it’s how many you feel really close to over time.”
This study was supported by the National Institutes of Health, the Mind, Body, Brain and Health Initiative of the John D and Catherine T MacArthur Foundation, the Norman Cousins Center at UCLA, the John Templeton Foundation, and the James B Pendelton Charitable Trust.
Although small, this is remarkable and shows how much nature not only abhors a vacuum, but also dislikes isolation. We are social animals and anything that gets in the way of that will likely lead to a very poor outcome.
It is fitting that Norman Cousins, for whom the UCLA center is named, had this to say:
“The eternal quest of the individual human being is to shatter his loneliness.”
“The most terrible poverty is loneliness and the feeling of being unloved.”
-Mother Teresa of Calcutta (Albanian-born Indian Nun, Humanitarian and, in 1979, Winner of the Nobel Peace Prize, 1910-1997)
The Curse of Crystal Meth

I have the dubious distinction of living in a part of the United States with one of the highest rates of methamphetamine abuse in the country. Around here most of the first time users are teenage girls who are trying to lose weight.
In the last few years the spread of methamphetamine abuse across the United States has been as rapid as it has been alarming. Until about six years ago, methamphetamine use was seen mostly in the western and rural United States. Then it jumped over the Mississippi and continued its demonic march to the sea and Georgia has been hit like a ton of bricks.
Not only can crystal met ravage the brains of users, they can get a wide range of physical problems including inflammatory and immune problems throughout the body.
Methamphetamine abuse has now expanded rapidly throughout the rest of the country and across different ethnic groups. According to the 2005 National Survey on Drug Use and Health it is estimated that 10.4 million Americans ages 12 or older have used methamphetamine at least once in their lifetimes for non-medical reasons.
There is a new and important study from the Scripps Institute that has shown that long-term methamphetamine use changes circulating proteins in drug users, causing aberrant immune responses. As a result, increased levels of pro-inflammatory cytokines – proteins that are involved in immune responses – may initiate a previously unrecognized molecular mechanism for the development of cardiovascular disorders including vasculitis, an inflammation of the blood vessels.
It appears that methamphetamine can add sugars (a.k.a. “glycate”) proteins. The researchers found that the immune system responds dramatically to this methamphetamine-induced glycation, which may lead to vascular inflammation. There was a direct relationship between methamphetamine intake and the level of circulating antibodies in animal models. This immune response, coupled with antibodies binding to methamphetamine, might make the drug less biologically available leading to an increased need for higher and higher doses, a problem found among chronic methamphetamine users.
The resulting glycated proteins are called advanced glycation end products (AGEs) that modify the function of proteins and are associated with a number of diseases including diabetes and Alzheimer’s disease.
Methamphetamine-AGE proteins not only increased antibody production, but also were strong enough to overcome the drug’s natural immunosuppressive qualities. Furthermore, a wide range of cytokines directly linked to AGE exposure were increased in rats that self-administered methamphetamine.
The study also showed that even limited daily access to the drug was enough to produce an over-expression of vascular endothelial growth factor which is a potent signaling cytokine involved in angiogenesis and vasodilatation.
If you know anyone tempted to dice with this vile toxin, ask them to have a look here.
T'ai Chi Ch'uan and Shingles

Shingles can be a particularly nasty problem, and treatment can be tough. It should be called herpes zoster, and it is caused by re-activation of varicella zoster virus (VZV) that causes chickenpox.
A new study from the Norman Cousins Center for Psychoneuroimmunology at UCLA, has shown that t’ai chi therapy can stimulate the immune system of patients with shingles to levels comparable to those achieved using a vaccine against VZV.
It was a controlled trial in which the researchers randomized 112 healthy adults aged 59 to 86, who had a history of varicella infection, to Tai Chi Chih (TCC, a simplified, standardized form of tai chi) or health education (HE) for 25 weeks. After 16 weeks of intervention, subjects were vaccinated against VZV. The results of blood tests showed that TCC alone increased immunity against VZV by an amount comparable to that induced by varicella vaccine in the HE group.
It was interesting that the effects of the two were additive; TCC, together with varicella vaccine, produced a substantially higher level of immunity against VZV than vaccine alone, raising it to levels usually observed in adults 30 years younger.
The tai chi group also showed significant improvements in scores for physical functioning, bodily pain, vitality, and mental health.
Regular readers will recall another report from this research group, indicating that TCC reduced the activity of the sympathetic nervous system. The two studies both show that there is something special going on: the practice does not only calm the mind and body, it also regulates parts of the body that are normally beyond voluntary control.
There are clearly plenty of reasons for taking up t’ai chi, though now we shall have to see whether other forms of t’ai chi can achieve the same results.
T’ai Chi Ch’uan and Diabetic Health

Regular readers will know that I am a great fan of t’ai chi ch’uan and qigong. I have been recommending them to people for years and even taught it for a while.
I have also been very interested in metabolic problems, particularly insulin resistance and diabetes.
So I was intrigued to see a study from Taiwan that was just sent to me.
The trial involved thirty-two people with type 2 diabetes mellitus who participated in three hour-long tai chi sessions once a week for 12 weeks. The conclusions were that practicing t’ai chi might help improve one component of immune function and also improve the control of blood glucose.
The researchers found statistically significant reductions in levels of glycosylated (glycated) hemoglobin in the blood of participants, indicating improved long-term blood glucose control. Glycosylated hemoglobin or HbA1c reflects the average blood glucose over the last 8-12 weeks, implying that the improvement must have been quite swift.
They also found increased numbers of regulatory and killer T cells. This may be important: people with diabetes are at considerably increased risk of getting infections.
It is even more impressive that the study was published in the journal Diabetes Care, that is known for its exacting standards.
If you or a loved one has diabetes, you may want to think about taking up t’ai chi.
Good luck!
Sleep Deprivation

When I was a young doctor we used to work absurdly long hours: for more than three years I worked every other night and every other weekend. It was not uncommon to be on your feet for three at a time. It is a wonder that we didn’t die or make more mistakes.
We know that sleep deprivation is not healthy, but we are only now beginning to find out just how damaging it can be. One of the biggest problems is that sleep deprivation interferes with the normal functioning of the immune system.
I saw an interesting paper (NR619) at the 2007 Annual Meeting of the American Psychiatric Association in San Diego last month.
A team from Korea took sixteen healthy volunteers and made them stay awake for 48 hours. They found that even this relatively short period of sleep deprivation produced some impressive effects on the body and the mind:
- Thyroid hormone levels rose
- The speed and accuracy of reaction times fell
- Blood glucose and protein levels rose, and there were disturbances in several liver function tests
- White blood counts increased
- There was a slight fall in immunoglobulin levels
We already know that insufficient sleep is associated with insulin resistance and weight gain, and it is likely that these are mediated by a rise in inflammatory mediators in the blood.
It is remarkable how quickly the effects occur.
And how pleased I am that young doctors no longer have to tolerate those incredibly long shifts.
Some things have changed for the better!
A Promising New Treatment for Lupus Kidney Disease
Systemic lupus erythematosus (SLE) is an out-of-control, malignant attack on the body by its own immune system. It can be a horrible illness that may affect virtually every organ of the body. One of the worst things is that it can lead to renal (kidney) failure. Until now, the treatments of SLE have been either symptomatic or "disease-modifying." The second is what we really want: to prevent the illness from progressing. But it has been very difficult to do that, and I have seen some real tragedies in my career.
We now have a new approach that highlights a new approach to illness in general. Students are usually taught that there are diagnostic tests for illnesses like SLE or prostate cancer. The idea of using the tests for treatment is fairly new. So one of the proteins that goes up in prostate cancer becomes the target for treatment.
But what about SLE?
SLE is a chronic inflammatory disease in which the body produces antibodies against the nuclear components of its own cells. The most worrying are antibodies to double-stranded DNA (dsDNA). These antibodies can be triggered by genetics, environmental factors like sunlight and some drugs.
The antibodies attack the body’s cells and tissue, resulting in inflammation and tissue
damage. SLE can affect any part of the body, but most often damages the heart, joints, skin, lungs, blood vessels, liver, kidneys and nervous system.
La Jolla Pharmaceutical Company just announced positive interim antibody results from its ongoing double-blind, placebo-controlled randomized Phase 3 trials of Riquent(R) (abetimus sodium). This is a drug candidate for SLE. Analyses of interim antibody data indicate that patients treated with 900 mg or 300 mg per week doses of Riquent had greater reductions in dsDNA antibodies than patients treated with 100 mg per week or placebo. The results showed a significant dose response when comparing all Riquent-treated patients to placebo-treated patients (p < 0.0001), and each Riquent dose group to the placebo dose group (p < 0.0015 for 100 mg, p < 0.0001 for 300 mg and 900 mg).
For people not used to looking at statistics, these are impressive data.
Clearly other analysts feel the same way: the price of the company’s shares went up 40% on the announcement.
We shall keep an eye on the development of this new medicine to see if it fulfills this early promise. At this moment the data are very exciting.
Here Comes the Sun: To Screen or Not To Screen?

I have been worried to see some people – all, I think, without scientific training – proclaiming that there is no need to protect ourselves against the sun because there is no evidence that sulight causes any health problems.
Ultraviolet radiation (UVR) from the sun has been part of the environment since the first cells began to form. When we discuss the effects of UVR on human health and the environment, the range of UV wavelengths is often subdivided into:
- UVA (400–315 nm), also called Long Wave or “blacklight”
- UVB (315–280 nm), also called Medium Wave
- UVC (< 280 nm) also called Short Wave or “germicidal”
The key questions are these:
Can sunlight cause health problems?
Do the benefits of sunlight outweigh their risks?”
UVB is required for the conversion of 7-deoxycholesterol to vitamin D, (the sunshine vitamin!) which is critically important in the maintenance of healthy bones, although there may also be another mechanism by which vitamin D is generated in the body. As we have seen research is making clear that vitamin D has other potential roles in the maintenance of human health. Low levels of vitamin D have been linked to:
- Rickets
- Osteomalacia
- Osteoporosis
- Maintaining the integrity of cell membranes
- Type 2 diabetes mellitus
- Schizophrenia
- Multiple sclerosis
- Pre-eclampsia (hypertension and accompanying problems during the late stages of pregnancy)
- Some types of cancer
- Fibromyalgia-like pains
- Immune deficiency: Africa Americans do not generate enough of a protein needed to ward off tuberculosis. Why? Because the protein needs vitamin D to be activated, and dark skin is inefficient at absorbing and converting UVR. It may also be that we see epidemics of colds and flu in the winter because that is when we have low levels of vitamin D, which allows the viruses to overwhelm our immune defenses.
This does not necessarily mean that taking extra vitamin D will ward off all of these problems.
In the days before the Industrial Revolution, unless we lived in the frozen North, we had no trouble in getting the amount of vitamin D that we needed. In most of the United States, during the summer months, 10-15 minutes outdoors at midday will generate around 10,000 international units (IU’s) of vitamin D in an average fair-skinned person. This is far in excess of the government’s dietary recommendations of 200 IU’s/day in people up to age 50, 400 IU’s up to age 70 and 600 IU’s in people over 70. Not surprisingly many experts – me included – believe and have provided evidence that these daily requirements are much too low. (Have a look at the comments here.)
Of course many of us do not spend much time outside and don’t take in as much in the way of vitamin D containing foods – such as milk and salmon – as we should. I’ve seen evidence to suggest that we in Atlanta are probably at the Northernmost point in the United States were we could hope to get enough sunshine and therefore vitamin D from modest winter exposure to the sun.
Recent data has suggested that if you spend no time at all in the sun, then you may need as much as 4,000 IU’s of vitamin D/day, though that figure has not yet been widely accepted.
Exposure to UVR, whether of solar or artificial origin, also carries potential risks to human health. UVR is a known carcinogen and excessive exposure, at least to the solar radiation in sunlight, increases the risk of cancer of the lip, basal cell, and squamous cell carcinoma of the skin and melanoma, particularly in fair-skinned populations. There is also evidence that solar UVR increases risk of several diseases of the eye, including cortical cataract, some conjunctival neoplasms, and perhaps also melanoma of the eye.
We have good data for the existence of a threshold amount of UV-B exposure that may lead to the formation of cataracts. The amount needed to cause cataracts depends in part on the amount of pigment in the eye, so albino rats get cataracts with much lower exposures to UV-B.
So what to do?
Sunlight has a definite benefit in preventing or treating many clinical problems and it is no surprise that after 3000 millennia we are adapted to make use of the sun’s largesse. What is less easy to understand is why an excess of sunlight can cause so many problems, unless it is our hairlessness and environmental change that has lead to a loss of the ozone layer.
Some years ago it was suggested that sunscreens may themselves cause skin cancer, but the data has shown that to be false. Indeed modern sunscreens almost certainly reduce melanoma risk.
So how do we balance the positive and negative effects of sunlight? A recent review precisely reflects my own thinking:
- We need some sunlight
- Depending on where you live, you need only a few minutes each day
- Sunscreens confer protection on the skin without blocking all the health benefits
- If you have a medical reason for avoiding sunlight, then your health care provider should measure your vitamin D status.
Toxoplasmosis and Behavior
Last August I wrote an article about some extraordinary new evidence implicating Toxoplasma gondii in some psychological and psychiatric illnesses. Latent infection with
Toxoplasma gondii is amongst the most prevalent of human infections and it
had been generally assumed that it is asymptomatic unless there is
congenital transmission or reactivation because a person has an immune system that has become depressed or compromised. That assumption is being completely re-evaluated.
The article generated some extremely interesting correspondence and some spirited discussions.
Here is a very insightful letter from a physician:
Dear Dr. Petty,
I thought about the concept of psychological illness caused by a virus or other organism. I was wondering what would be the mode of dispersion of such a virus. Upper respiratory tract infections, skin and gastrointestinal infections spread by cough, by touch and hand to mouth respectively. How would such a brain virus or protozoal organism promote itself? Of course it could be by the above methods but it seems that there should some way that the specific disease process is connected to a behavior that helps it to spread itself.
Then I got to thinking; diseases have learned physical ways to disseminate themselves, I wonder if a disease could change behavior to promote it’s own dissemination and survival? I imagine that if that were true, people with the flu would be sociable, people with infectious diarrhea would be sociable and hungry, people with AIDS would have increased libido. I haven’t yet seen any data for this. Although I’ve always felt that there was one disease that did alter behavior in a way that is conducive to disseminating itself, and that is rabies. The host goes from being docile, to seeing all others as the enemy. He then attacks them, bites them and thus passes on the organism. A true mind altering virus, although it’s psychology works better with animals than with people. Do you think that there are other diseases that spread purely by behavior, that cause the host to seek out the next host and not just pass the disease from one to another just due to proximity?
This was my response:
What great questions!
And believe it or not, there’s quite a lot of empirical research on these very topics.
There is a whole textbook on the behavioral effects of parasites edited by Janice Moore entitled Parasites and the Behavior of Animals. Here’s an interesting one: rats and mice are hard wired to avoid cats. Millions of years of programming have ensured that Tom’s very presence would send Jerry packing. Cats carry Toxoplasma gondii and if mice or rats become infected with it, usually by eating cat poop, they lose their fear of felines. So now Tom can have lunch at his leisure.
I’ve also talked about the way in which people with creativity and schizotypal personality disorder (i.e. carriers of genetic risk) tend to be promiscuous, while people with schizophrenia have fewer children. Both groups tend to get more sexually transmitted diseases than the general population. It would be tempting to think that toxoplasmosis can be spread that way, however there’s a 32-year old study in German that showed that Toxoplasma was not transmitted by intercourse. However, cytomegalovirus, a common partner to Toxoplasma may be. And both modulate dopamine activity in the regions of the brain involved in salience.
I have done a very detailed literature search encompassing papers written in all the languages that I can read, and have not been able to find any clear evidence of behavior change induced by HIV, influenza or infectious diarrhea: what interesting and important questions to research.
We do have some more data confirming the effects of Toxoplasma infections on the behavior of rats: they become less anxious and therefore do not respond to environmental threats as quickly as uninfected rodents. An antipsychotic medication (haloperidol), a mood stabilizer (valproic acid) and two chemotherapeutic agents – pyrimethamine or Dapsone – have all been shown to prevent the development of Toxoplasma-induced behavioral change.
Another recent study from the Departments of Parasitology, Microbiology and Zoology, Charles University, the Centre of Reproductive Medicine and GynCentrum, in the Czech Republic also speaks to the significance of latent Toxoplasma infections: the presence of the parasite in the blood of pregnant women increases their chance of giving birth to boys. The increased survival of male embryos in infected women may be explained by Toxoplasmosis infections modulating and suppressing the immune system.
If Toxoplasma plays a part in the development of some psychiatric illnesses, yet a high proportion of the population carries it without any problems, one obvious question is what activates it? Environmental stress might, perhaps, cause the Toxoplasma to become reactivated and play a part in the development of specific psychiatric symptoms.
This story is continuing to develop and I am going to watch it closely. If it is confirmed, it could open up some brand new avenues for helping treat and perhaps even prevent some types of psychiatric illness.






