A New Approach to the Diagnosis and Treatment of Depression

Although textbooks and pharmaceutical company literature often claim that the biological component of depression has been clearly defined, the fact is that we still have no certain knowledge about the molecular and biochemical disturbances in depressive disorders. Furthermore, our theories of how antidepressants are constantly being revised, and it is now thought likely that these drugs have several mechanisms of action.
There is an interesting study from the University of Illinois at Chicago College of Medicine and Maryland Psychiatric Research Center in Baltimore in today’s issue of the Journal of Neuroscience.
They have discovered that a change in the location of a protein in the brain could serve as a biomarker for depression. This is exceptionally important, since it may give us a simple and rapid laboratory test to identify patients with depression and, more importantly, to predict clinical response to specific antidepressants.
Over the last few years this same team of researchers, and others around the globe, have been examining a protein named Gs alpha that activates adenylyl cyclase. Adenylyl cyclase is a link in signal transduction that is in part responsible for the action of neurotransmitters including serotonin. Instead of just looking at the biochemical properties of the protein, they have also been looking at the way that it moves in the cell membrane, which in turn impacts the way in which neurotransmitters act on cells.
In both rats and cultured brain cells, Gs alpha changes its location in response to antidepressants, moving out of lipid “rafts” in the cell membrane, to areas of the membrane that allow more efficient communication among membrane components responsible for the action of neurotransmitters. Both antidepressant and antipsychotic drugs have been shown to concentrate in these lipid rafts.
In this new study, brain samples from depressed people who had committed suicide were compared with controls who had no history of psychiatric disorders. Although the total amount of Gs alpha was the same in the depressed and non-depressed, in people with depression, Gs alpha was stuck in these lipid “rafts.” Therefore the protein is unable to do its job of mediating the action of neurotransmitters. Antidepressants have the opposite effect, moving it to regions of the membrane where it can do its work. The localization of other G proteins was not different.
This is such a robust finding, that identifying the location of Gs alpha in the cell membrane may provide an objective diagnosis of depression and second, whether someone is responding to the chosen antidepressant therapy.
The senior author in this research is Mark Rasenick, who is distinguished university professor of physiology and biophysics and psychiatry at the University of Illinois. He described the lipid “rafts” and the importance of the findings like this:
“These “rafts” are thick, viscous, almost gluey areas, that either facilitate or impede communication between membrane molecules… When Gs alpha is caught in these lipid raft domains, its ability to couple with and activate adenylyl cyclase is markedly reduced. Antidepressants help to move the Gs alpha out of these rafts and facilitate the action of certain neurotransmitters.”
He goes on to say,
“This test could serve to predict the efficacy of antidepressant therapy quickly, within four to five days, sparing patients the agony of waiting a month or more to find out if they are on the correct therapeutic regimen.”
The findings may also help explain two old puzzles:
- Why do antidepressants take so long to work?
- Why do such chemically different compounds produce similar clinical effects?
We are going to need a load of further studies to confirm and expand these findings, and to examine the clinical utility of the test. But it’s a great start.
Are Antidepressants Effective?

An important story has been flashed around the world, but unfortunately some of the interpretations of the story have been intemperate. In a study published in PLOS Medicine a team of researchers from the University of Hull team concluded the drugs actively help only a small group of the most severely depressed. They based this on a meta-analysis of all clinical trials submitted to the US Food and Drug Administration (FDA) for the licensing of the four new-generation antidepressants for which full datasets were available.
The researchers reviewed data on 47 clinical trials, both published clinical trial data, and unpublished data secured under Freedom of Information legislation.
They focused on four antidepressants: fluoxetine (Prozac), venlafaxine (Effexor), nefazodone (Serzone) and paroxetine (Paxil).
Many of the reports in the media have taken this research to mean that antidepressants are no better than placebo. That is not the case. The medications can be very effective and even life saving in people with severe depression. However, the effect in people with mild depression is no greater than placebo.
What this tells us is that the over-prescription of antidepressants for normal variations in mood is probably not justified. We are all allowed to be miserable from time to time, but that does not mean that we need to take medications.
Not surprisingly, some of the manufacturers have strongly disputed the findings.
The biggest worry after reading some of the news reports is that some people might stop their medications abruptly, and that can cause many problems. And some folk really do need to be on the medications and stopping them without clear guidance can be very risky.
Mold, Dampness and Depression

It matters where you live.
I have lived or stayed in many countries, and there is no doubt that some places are a lot more congenial than others. I don’t just mean a beach in Thailand compared with the North of Scotland in winter. Some places just make you feel better. There are many physical, psychological, social and subtle reasons, but here is a relatively new one.
There is an important paper in this month’s issue of the American Journal of Public Health looking at the possibility of a link between dampness and mold in the home and clinical depression.
Molds are fungi that are found in many environments but most of them grow best in warm, damp, and humid conditions. Therefore, dwellings that have problems with damp also commonly have problems with mold. Although the physical health consequences of living in a damp and moldy dwelling are quite well known, the effect of living in such an environment on mental health has not.
Some of the known health problems associated with high levels of airborne mold spores include:
- Allergic reactions
- Asthma
- Irritations of the eyes, nose and throat
- Sinus congestion and other respiratory problems
- In people with with weakened immune systems, inhaled mold spores may germinate, attaching to cells along the respiratory tract
- Immunocompromised individuals exposed to high levels of
mold may get a systemic fungal
infection - Infections of the digestive tract, lung and skin
The researchers used survey data from 8 European cities. They created a dampness and mold score from resident- and inspector-reported data. Depression was assessed using a validated index of depressive symptoms.
The results showed that dampness and mold were associated with depression, independent of individual and housing characteristics. This association was independently mediated by perception of control over one’s home and by physical health.
This link is most likely because of the psychological and physiological consequences of living in poor housing conditions. But there could also be a direct pathological effect of mold itself.
Optimism and the Brain

Humans have a wonderful ability to expect positive events in the future, even when there is no shred of evidence to support them. One of the key components of resilience is optimism. Though there is data to show that there is a genetic contribution to optimism, it is also a psychological attribute that can flow from life experiences as well as attitude that can be developed. Though the motivational coaches who tell us that putting on a happy face will make you happy and optimistic are probably overstating the truth! A lack of optimism is often a sign of clinical depression so learning more about it, is not just an academic exercise.
New research just published in the journal Nature indicates that there are two regions of the brain linked to optimism.
The team from New York University and University College, London, says that the act of imagining a positive future event, for example winning an award or receiving a large sum of money, activates two brain areas: the amygdala and the rostral anterior cingulated cortex (rACC). The finding ties in with earlier studies that suggested that these brain regions malfunction in depression. (1,2)
The investigators first measured how optimistic 15 volunteers were using a standard questionnaire. They were then scanned using functional magnetic resonance imaging (fMRI) while reflecting on one of a number of potential scenarios.
In one part of the trial, subjects followed specific instructions to recall a negative event in the past, such a funeral that they had attended in the past five years. In another experiment they had to imagine what it would be like to be involved in a car crash in the near future. At other points in the study subjects had to reflect on positive events such as winning an award in the past or receiving a large sum of money in the future.
Reflecting on both past and future events activated the amygdala and the rACC regions of the brain. However, positive events, and particularly those imagined in the future, generated a significantly larger response in these regions than reflecting on negative events.
When imagining happy events, the more pessimistic subjects in the trial had less activation of these brain areas than their optimistic counterparts when imagining happy events.
For some time now, many researchers have assumed that the amygdala and rACC are only involved in negative thoughts and negative reactions, but this research indicates that they have an important role in signaling cheerful thoughts. And, what is more, these are also regions of the brain that have been implicated in depression. Previous research has suggested that patients with depression have decreased nerve signaling and fewer cells in the rACC and amygdala.
Is this why people with depression find it so hard to generate positive thoughts?
This is important work that will likely have a great many practical applications.
“Children are born optimists and we slowly educate them out of their heresy.”
–Louise Imogen Guiney (American-born English Poet, 1861-1920)
“Although the world is full of suffering, it is full also of the overcoming of it.”
–Helen Keller (American Blind and Deaf Swedenborgian Philosopher, 1880-1968)
“No man is so old as not to think he can live one year more.”
–Marcus Tullius Cicero (Roman Political Figure and Orator, c.106-43 B.C.E.)
“The way to become happy
Is to think
And to feel
That the very best is yet to come.”
–Sri Chinmoy (a.k.a. Chinmoy Kumar Ghose, Indian Philosopher and Spiritual Teacher, 1931-2007)
Sleep Deprivation and Emotional Instability

Most of the time we are in control of our moods, rather than our moods being in control of us. One of the main things that we learn as we get older is not simply to damp down our emotional reactions, but to make them “contextually relevant:” we produce the right emotional response for the right situation. Yet we also know that there are exceptions: times when our emotions over-run any attempts at our control.
Second, we all know that sleep deprivation can be a Bad Thing. It is known to impair a range of mental and physical activities, including immune function, metabolic control and many cognitive processes, including learning and memory.
It has long been suspected that sleep deprivation can have significant effect on mood. Many of us feel irritable and distractible if we haven’t slept enough, and you may have had the experience of being up all night and feeling a little bit “high” in the morning. It has also been known for centuries that mood disorders are very commonly associated with sleep disturbances, and sleep disturbance is often the first sign that someone with mood problems is running into trouble. So mood and sleep must be linked in some way.
Despite these common observations, there has never been that much empirical evidence for the impact of sleep deprivation on mood, and in particular the effects of sleep deprivation on the brain.
An important new study by researchers from Harvard Medical School and the University of California at Berkeley has just been published in the journal Current Biology, and it is beginning to fill in some of the gaps in our knowledge.
The amygdala is known to be involved in processing of emotionally salient information, particularly unpleasant or aversive stimuli. In mature individuals, the emotional centers of the brain are usually controlled and modulated by an array of connected systems, mainly in the frontal regions of the brain. One particularly important part of the frontal lobes that is involved in controlling the amygdala is the medial-prefrontal cortex (MPFC). Under normal conditions the MPFC is supposed to exert an inhibitory, top-down control of the amygdala, so that we only generate appropriate emotional responses.
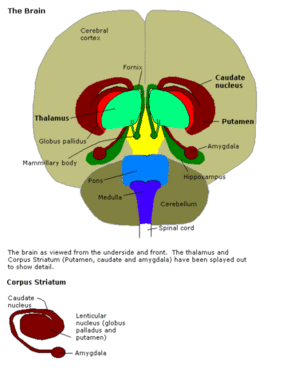
The scientists worked with 35 volunteers who were deprived of sleep for 35 hours. Blood flow can be used to deduce which specific regions of the brain are active. The researchers used functional magnetic resonance imaging (fMRI) to examine the blood flow – and therefore activity – in the brains of the volunteers in real time, both during and after sleep deprivation.
After going without sleep, the participants were asked to look at images that were designed to trigger angry or sad emotional responses. The investigators discovered that the amygdala showed 60% higher reactions to the images compared with people who are not sleep-deprived.
This is an extraordinarily large effect and implies that sleep deprivation knocks out the normal control mechanisms in the frontal lobes so that the sleep-deprived brain reverts to a more primitive pattern of activity. As a result we become unable to put emotional experiences into context and produce controlled, appropriate responses.
If we needed any more reasons to get a good night’s sleep, this one is very powerful. It also re-iterates something very important: if you or a loved one have had problems with mood, anger or anxiety, it is essential to watch your sleep pattern. Any change may be a harbinger or trouble, and is an excellent early warning that you or they need a hand to make sure that things stay on an even keel.
“Your brain shall be your servant instead of your master, you will rule it instead of allowing it to rule you.”
–Charles E. Popplestone (American Author of Every Man a Winner, 1936)
“Control your emotions or they will control you”
–Chinese Proverb
“For the uncontrolled there is no wisdom, nor for the uncontrolled is there the power of concentration; and for him without concentration there is no peace. And for the unpeaceful, how can there be happiness?”
–Bhagavad Gita (Ancient and Sacred Sanskrit Poem Incorporated into the Mahabharata)
“He who controls others may be powerful, but he who has mastered himself is mightier still.”
–Lao Tzu (Obscure Chinese Philosopher, Founder of Taoism and Alleged Author of the Tao-Te Ching, c. 604-c. 531 B.C.E.)
“ . . . let every man be swift to hear, slow to speak, slow to wrath.”
–The Bible, James 1:19
“When angry, count ten before you speak; if very angry, a hundred.”
–Thomas Jefferson (American Writer, Philosopher, Politician and, from 1801-1809, 3rd President of the United States, 1743-1826)
Chocolate, Comfort Foods and Depression

Most people have done a bit of comfort eating from time to time: candies and chocolates are usually the favorites. That’s not a coincidence. Not only do they taste good, but chocolate also contains chemicals that may improve mood, and sugar can have an indirect impact on the uptake of specific amino acids into the brain, where they go on to form the chemical neurotransmitters involved in inter-cellular communication and learning.
On the more serious side, some types of mood disorders, particularly seasonal affective disorder, premenstrual syndrome and the so-called “atypical depression” are often associated with quite sever cravings for chocolate.
So I was very interested to see a paper from colleagues in Australia in this month’s issue of the British Journal of Psychiatry.
Gordon Parker and Joanna Crawford examined links between chocolate craving in people who are depressed and both personality style and atypical depressive symptoms, with a web-based questionnaire completed by nearly 3000 individuals reporting clinical depression.
People accessing a mood disorder consumer information website (http://www.blackdoginstitute.org.au) were invited to participate in an online survey of lifetime treatments for a depressive episode, together with some interesting evaluation tools.
Half of the respondents said that they craved chocolate, and the number was slightly higher in women. They said that they felt that chocolate helped with depression, anxiety and irritability. The ones who said that chocolate helped were more likely to score higher on a “neuroticism” scale, particularly irritability and rejection sensitivity.
Five years ago the same team found that atypical depression was associated with a personality that was especially sensitive to rejection, and also tended to be linked with several symptoms – including food cravings – that tie in with behaviors aimed to try and make us feel better and to maintain internal balance.
The results suggest that people with certain personality styles derive personal benefit from comfort eating. Some research has linked carbohydrate craving to the opioid system in the brain, and it is possible that munching on chocolate may be an example of genuine self-medication. People eat to chocolate to calm down their ability to feel emotional distress.
The trouble is, of course, that although chocolate is yummy and may even be therapeutic, too much can be a bad thing. Weight problems are common in people with chronic depression, especially the “atypical” type.
“Chocolate causes certain endocrine glands to secrete hormones that affect your feelings and behavior by making you happy. Therefore, it counteracts depression, in turn reducing the stress of depression. Your stress-free life helps you maintain a youthful disposition, both physically and mentally. So, eat lots of chocolate!”
–Elaine Sherman (American Culinary Expert, Teacher and Writer, 1938-2001)
“Look, there’s no metaphysics on earth like chocolates.”
–Fernando Pessoa (Portuguese Poet, 1888-1935)
A Virus Linking Depression, Aging and Heart Disease

We have known for a long time that there are close links between depression, aging and heart disease, but the nature of the link has remained elusive. Most of the smart money has been on inflammation, but there could be other candidates.
New research in the journal Brain, Behavior and Immunity has linked an increase in two inflammatory proteins in the immune system with a latent viral infection and proposes a chain of events that might accelerate cardiovascular disease. It is possible that the same process may be involved in a number of other ailments that can afflict us, as we get older. The findings also suggest that chronic depression may play a key role in initiating the cascade that can lead to the development of coronary artery disease.
It has been known for some time that increased levels of the proinflammatory cytokines, TNF-α and IL-6, predict mortality and morbidity. High levels of each of them are found in the plasma and in atherosclerotic lesions of people with cardiovascular disease.
The levels of IL-6 in the body increase as the immune system ages. Some of the IL-6 is generated by immune cells – macrophages – that go to the site of an infection or injury. Earlier work by the team also showed that increases in psychological stress and depression could substantially raise the levels of IL-6 and TNF-α in the body.
Increased stress and depression can also trigger latent viruses to reactivate and begin reproducing inside cells. The viruses of greatest interest are some herpes viruses such as the Epstein-Barr virus (EBV). We know that up to 90% of the people in North America have been infected by EBV by the time they are adults.
If EBV begins to multiply in cells in the body, it produces a protein called dUTpase that, in turn, can stimulate macrophages to make yet more IL-6.
The researchers developed a model to test these linkages by using endothelial cells that line the inside of veins in umbilical cord tissue. I spent years working with these cells myself, and they provide an excellent substrate for examining vascular responses and the interaction between blood vessels and macrophages when exposed to the virus as well as the dUTpase protein.
As expected, the production of IL-6, as well as TNF-a, were increased just as they would be as part of the inflammatory process in the body. Such chronic incidents of inflammation are integral to the onset of atherosclerosis and an array of other diseases.
This work suggests a new way of thinking about how vascular diseases develop. We carry around these latent herpes viruses in our bodies virtually all our lives and periodically they can hurt us as we age, develop depression or, perhaps a nutritional imbalance.
Taken together with the recent data on the physical effects of loneliness, if you want to live a long and healthy life:
- Watch you mood: depression can kill you
- Stay socially engaged: loneliness can be fatal
- Maintain a balanced diet
- Take some physical exercise every day
- Learn – and practice! – some simple stress management techniques. You can obtain some at RichardGPettyMD.com
Sleep and Your Heart

The amount of sleep a person gets affects his or her physical health, emotional well-being, mental abilities, productivity and performance. Recent studies associate lack of sleep with serious health problems such as an increased risk of depression, obesity, cardiovascular disease and diabetes.
There was some interesting research presented at SLEEP 2007, the 21st Annual Meeting of the Associated Professional Sleep Societies in Minneapolis in the middle of June.
One study that caught my eye was conducted by Siobhan Banks of the University of Pennsylvania School of Medicine. The research was based on preliminary analysis of 39 subjects, each of whom participated in a laboratory-controlled chronic sleep restriction protocol. The subjects underwent two nights of baseline sleep followed by five hours of sleep restriction. The results showed a statistically significant decrease in the heart rate variability after just five nights of sleep restriction.
We already know that a reduction in heart rate variability may occur in several cardiological and non-cardiological diseases, and it is usually a harbinger of a poor outcome.
This work may provide the mechanism for why short sleep duration is associated with a heightened risk of heart and other circulatory problems.
The amount of sleep a person gets affects his or her physical health, emotional well-being, mental abilities, productivity and performance. Recent studies associate lack of sleep with serious health problems such as an increased risk of depression, obesity, cardiovascular disease and diabetes.
So if confirmed, the take home message is that sleep deprivation has a negative effect on a person’s cardiac activity and that may in turn increase the risk of cardiovascular disease and mortality.
Emotions and Recovery from Hip Surgery

A patient’s emotional state plays a significant role in his or her recovery from hip surgery according to research from Saint Louis University. This research was particularly interesting because the researchers were not looking for a link.
Orthopedic surgeons typically use two tests to determine if a patient has recovered from hip surgery: one is a clinical measure of hip function and the second is a patient questionnaire that looks at a number of factors that may play a role in the overall success of the surgical procedure. Originally the research was simply designed to see if the two measures, the clinical one that has been in use for decades, the other, a new subjective scale, correlated in some way.
The clinical test found good-to-excellent results, while the self-test taken by the same patients showed significantly worse recovery. The disparity could be explained by a section of questions on the self-test that are not addressed by the clinical test: those dealing with emotional well-being. After post-operative mobility, the patient’s emotional status was the most important factor in determining how well he or she thought recovery was going.
It is common for doctors to think that patients are doing well because they have achieved a good technical result. But if the patient is still miserable, depressed and in pain, we should not congratulate ourselves on a job well done.
Yet a great many people are denied the help that they need. For instance they may have already had depression or they may be depressed because of pain and immobility. It does not really matter which came first. If the psychological aspects of the illness or the surgery are not addressed, people are not likely to recover. The same goes for having poor nutrition or poor social supports.
The whole point of Integrated Medicine is to address every aspect of a person: physical, psychological, social, subtle and spiritual.
This study provides further evidence that if we only look at the physical aspects of a problem or an intervention, we are going to miss the boat.
Mindfulness and Depression

Mindfulness meditation has rightly been receiving a lot of attention recently. It is quite simply a technique in which you become intentionally aware of your thoughts and actions in the present moment, non-judgmentally. Though originally a Buddhist technique, it is something that can be practiced by anyone, and there are, in fact, similar techniques that have been developed by Christian mystics and Sufis.
It has recently been discovered that some of the techniques that were developed so that a mystic or meditator could carry on without distraction, may also have value in treating clinical problems. After all, if a group of people has spent a thousand years developing tools and techniques for managing the mind, it might be a good idea to see what they have discovered!
There have recently been several excellent books on the use of mindfulness in the management of depression:
The Mindful Way Through Depression
Relaxation, Meditation and Mindfulness
Mindfulness and Acceptance: Expanding the Cognitive-Behavioral Tradition
This whole field was moved forward by some research from San Francisco (NR822) that was presented at the end of May at the 2007 Annual Meeting of the American Psychiatric Association in San Diego. The researchers used Mindfulness-Based Cognitive Therapy (MBCT) in a group of 53 people with treatment resistant depression.
MBCT is based on the Mindfulness-based Stress Reduction (MBSR) eight-week program that was developed by Jon Kabat-Zinn in 1979 at the University of Massachusetts Medical Center. Research has show that MBSR can be enormously empowering for people with chronic pain, hypertension, heart disease, cancer, and gastrointestinal disorders, as well as for psychological problems such as anxiety and panic.
Mindfulness-based Cognitive Therapy grew from this work. Zindel Segal, Mark Williams and John Teasdale adapted the MBSR program so that it could be used for people who had suffered repeated episodes of depression.
The results of the study presented in San Diego showed that MBCT was effective in reducing depression when compared to treatment as usual: what we call “TAU.” What seems to happen is that MBCT gives people a set of skills for detaching from the stream of depressive thoughts and feelings. As a result the symptoms decrease. Though the study will need to be expanded and replicated, this is clearly a fertile area for research.
This work is also interesting in the light of recent research showing that mindfulness training may improve the activity of some of the subsystems of the brain dedicated to attention, as well as helping some people with mental illness control their aggressive behavior. Mindfulness training may also help to reduce subjective reduces distress and improves positive mood states. It seems to be particularly good at reducing distracting and ruminative thoughts and behaviors.
And just for good measure, mindfulness may help some smokers quit.
“The purpose of meditation is not enlightenment, it is to pay attention even at extraordinary times, to be of the present, nothing-but-in-the-present, to bear this mindfulness of now into each event of ordinary life.”
–Peter Matthiessen (American Naturalist and Writer, 1927-)
“Meditation is not to escape from society, but to come
back to ourselves and see what is going on. Once there is
seeing, there must be acting. With mindfulness, we know
what to do and what not to do to help.”
— Thich Nhat Hanh Vietnamese Buddhist Monk, 1926-)
“Conscious means “having an awareness of one’s inner and outer worlds; mentally perceptive, awake, mindful.” So “conscious business” might mean, engaging in an occupation, work, or trade in a mindful, awake fashion. This implies, of course, that many people do not do so. In my experience, that is often the case. So I would definitely be in favor of conscious business; or conscious anything, for that matter.”
–Ken Wilber (American Philosopher, 1949-)






