A Virus Linking Depression, Aging and Heart Disease

We have known for a long time that there are close links between depression, aging and heart disease, but the nature of the link has remained elusive. Most of the smart money has been on inflammation, but there could be other candidates.
New research in the journal Brain, Behavior and Immunity has linked an increase in two inflammatory proteins in the immune system with a latent viral infection and proposes a chain of events that might accelerate cardiovascular disease. It is possible that the same process may be involved in a number of other ailments that can afflict us, as we get older. The findings also suggest that chronic depression may play a key role in initiating the cascade that can lead to the development of coronary artery disease.
It has been known for some time that increased levels of the proinflammatory cytokines, TNF-α and IL-6, predict mortality and morbidity. High levels of each of them are found in the plasma and in atherosclerotic lesions of people with cardiovascular disease.
The levels of IL-6 in the body increase as the immune system ages. Some of the IL-6 is generated by immune cells – macrophages – that go to the site of an infection or injury. Earlier work by the team also showed that increases in psychological stress and depression could substantially raise the levels of IL-6 and TNF-α in the body.
Increased stress and depression can also trigger latent viruses to reactivate and begin reproducing inside cells. The viruses of greatest interest are some herpes viruses such as the Epstein-Barr virus (EBV). We know that up to 90% of the people in North America have been infected by EBV by the time they are adults.
If EBV begins to multiply in cells in the body, it produces a protein called dUTpase that, in turn, can stimulate macrophages to make yet more IL-6.
The researchers developed a model to test these linkages by using endothelial cells that line the inside of veins in umbilical cord tissue. I spent years working with these cells myself, and they provide an excellent substrate for examining vascular responses and the interaction between blood vessels and macrophages when exposed to the virus as well as the dUTpase protein.
As expected, the production of IL-6, as well as TNF-a, were increased just as they would be as part of the inflammatory process in the body. Such chronic incidents of inflammation are integral to the onset of atherosclerosis and an array of other diseases.
This work suggests a new way of thinking about how vascular diseases develop. We carry around these latent herpes viruses in our bodies virtually all our lives and periodically they can hurt us as we age, develop depression or, perhaps a nutritional imbalance.
Taken together with the recent data on the physical effects of loneliness, if you want to live a long and healthy life:
- Watch you mood: depression can kill you
- Stay socially engaged: loneliness can be fatal
- Maintain a balanced diet
- Take some physical exercise every day
- Learn – and practice! – some simple stress management techniques. You can obtain some at RichardGPettyMD.com
The Curse of Crystal Meth

I have the dubious distinction of living in a part of the United States with one of the highest rates of methamphetamine abuse in the country. Around here most of the first time users are teenage girls who are trying to lose weight.
In the last few years the spread of methamphetamine abuse across the United States has been as rapid as it has been alarming. Until about six years ago, methamphetamine use was seen mostly in the western and rural United States. Then it jumped over the Mississippi and continued its demonic march to the sea and Georgia has been hit like a ton of bricks.
Not only can crystal met ravage the brains of users, they can get a wide range of physical problems including inflammatory and immune problems throughout the body.
Methamphetamine abuse has now expanded rapidly throughout the rest of the country and across different ethnic groups. According to the 2005 National Survey on Drug Use and Health it is estimated that 10.4 million Americans ages 12 or older have used methamphetamine at least once in their lifetimes for non-medical reasons.
There is a new and important study from the Scripps Institute that has shown that long-term methamphetamine use changes circulating proteins in drug users, causing aberrant immune responses. As a result, increased levels of pro-inflammatory cytokines – proteins that are involved in immune responses – may initiate a previously unrecognized molecular mechanism for the development of cardiovascular disorders including vasculitis, an inflammation of the blood vessels.
It appears that methamphetamine can add sugars (a.k.a. “glycate”) proteins. The researchers found that the immune system responds dramatically to this methamphetamine-induced glycation, which may lead to vascular inflammation. There was a direct relationship between methamphetamine intake and the level of circulating antibodies in animal models. This immune response, coupled with antibodies binding to methamphetamine, might make the drug less biologically available leading to an increased need for higher and higher doses, a problem found among chronic methamphetamine users.
The resulting glycated proteins are called advanced glycation end products (AGEs) that modify the function of proteins and are associated with a number of diseases including diabetes and Alzheimer’s disease.
Methamphetamine-AGE proteins not only increased antibody production, but also were strong enough to overcome the drug’s natural immunosuppressive qualities. Furthermore, a wide range of cytokines directly linked to AGE exposure were increased in rats that self-administered methamphetamine.
The study also showed that even limited daily access to the drug was enough to produce an over-expression of vascular endothelial growth factor which is a potent signaling cytokine involved in angiogenesis and vasodilatation.
If you know anyone tempted to dice with this vile toxin, ask them to have a look here.
Sleep and Your Heart

The amount of sleep a person gets affects his or her physical health, emotional well-being, mental abilities, productivity and performance. Recent studies associate lack of sleep with serious health problems such as an increased risk of depression, obesity, cardiovascular disease and diabetes.
There was some interesting research presented at SLEEP 2007, the 21st Annual Meeting of the Associated Professional Sleep Societies in Minneapolis in the middle of June.
One study that caught my eye was conducted by Siobhan Banks of the University of Pennsylvania School of Medicine. The research was based on preliminary analysis of 39 subjects, each of whom participated in a laboratory-controlled chronic sleep restriction protocol. The subjects underwent two nights of baseline sleep followed by five hours of sleep restriction. The results showed a statistically significant decrease in the heart rate variability after just five nights of sleep restriction.
We already know that a reduction in heart rate variability may occur in several cardiological and non-cardiological diseases, and it is usually a harbinger of a poor outcome.
This work may provide the mechanism for why short sleep duration is associated with a heightened risk of heart and other circulatory problems.
The amount of sleep a person gets affects his or her physical health, emotional well-being, mental abilities, productivity and performance. Recent studies associate lack of sleep with serious health problems such as an increased risk of depression, obesity, cardiovascular disease and diabetes.
So if confirmed, the take home message is that sleep deprivation has a negative effect on a person’s cardiac activity and that may in turn increase the risk of cardiovascular disease and mortality.
Can a Pain in the Neck Raise Your Blood Pressure?
A chance discovery at the University of Leeds in the United Kingdom may give credence to longstanding claims by chiropractors that treating pain and stiffness by adjusting the neck can also lower blood pressure.
In a study published in the Journal of Neuroscience Jim Deuchars and his team report finding connections between rats’ neck muscles and a specific region of the brain. Their findings indicate that the neck muscles could play a key role in controlling blood pressure, heart rate and respiration.
They found that nerves run from receptors in the neck muscles to a region in the brainstem called the nucleus tractus solitarius that is known to be involved in the control of autonomic nervous system. It seems likely that signals from the neck could play a key role in ensuring an adequate supply of blood to the brain as we change position, for instance standing up suddenly. If the signaling system fails we may run into problems with low blood pressure (postural hypotension) and difficulties with balance.
Although it is early days, and it is a long way from a rat study to understanding human physiology, the finding may do more than provide a tentative explanation for the chiropractic reports. It may also explain another puzzle: why some people with whiplash injuries get trouble with their blood pressure. On the other hand, there have been a number of studies that have shown that the practice of yoga may help control blood pressure. It had been assumed that it was simply a consequence of generalized relaxation, but perhaps it is more specific than that: could a soft flexible neck be important in maintaining a healthy blood pressure?
The best research studies are the ones that suggest more questions than answers: on that criterion this is a most important study.
The Causes and Consequences of Insulin Resistance
I have spent so much time talking about insulin resistance becuase it is one of the greatest medical threats facing the world.
It is estimated that approximately 33% of the adult population of the United States is insulin resistant, and if left untreated many will develop diabetes, hypertension and an array of other problems. It is an epidemic that is expected to swamp most health care systems around the world, yet sadly it may in most cases be preventable.
There is an enormous literature on insulin resistance. As of this afternoon there are almost 33,000 scientific papers on the subject.
I created this graphic to try and summarize the key points about insulin resistance: the main factors that may cause it, as well as the most important medical consequences.
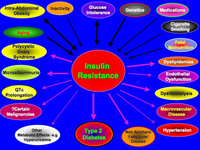
(Click on the graphic to expand it.)
The Main Causes of Insulin Resistance are:
- Aging
- Intra-abdominal obesity
- Inactivity
- Glucose intolerance
- Genetics
- Fetal malnutrition
- Cigarette smoking
- Some medications
The Main Consequences of Insulin Resistance are:
- Type 2 diabetes mellitus
- Hypertension
- Arteriosclerosis
- Polycystic ovarian syndrome
- Non alcoholic fatty liver disease
- Disturbances in the function of the vascular endothelium
- Elevations of triglycerides and cholesterol
- Disturbances of clotting
- Disturnaces in kidney function
- DIsturbances in one type of heart rhythm
- Elevated uric acide levels
- Some malignancies
This is probably not a complete list, but it gives you a very good idea of the reasons for looking for insulin resistance. Many – but not all – experts now recommend measuring insulin resistance in people at high risk of developing any of these medical problems.
We have good evidence that lifestyle changes can prevent the development of many of these dire consequences, so it is certainly something worth discussing with your health care provider.
Oral Health and Pointless Tests

I really like the Fox News Channel, but I sometimes worry about some of the medical advice that they dish out. The other morning I heard a dentist recommend that people should ask for a blood test to measure inflammation. She was saying that everyone should have the test, called C-Reactive Protein (CRP). This is really bad advice that is based on a fundamental misunderstanding of research data.
Yes, there is a link between dental disease and arteriosclerosis. And yes, there is a link between CRP and arteriosclerosis. But there is no good evidence that we should be measuring it on a routing basis.
The CRP Molecule
So what’s the problem about measuring CRP? If it is elevated, then what? There is no point in measuring anything at all unless you can take some action, or it guides prognosis. No good doctor would ever recommend treating a lab value. So if the CRP is elevated that would not just mean that it’s time to have a look at his or her pearly whites, it would mean a total body workup. There are dozens of causes for an elevated CRP. I know a lot about the topic: sixteen years ago I wrote one of the early scientific papers on CRP. It may go up if you have a fat tummy, have arthritis, allergies or if you are depressed, have fibromyalgia or irritable bowel syndrome. It also goes up as you get older, if you are physically inactive, or if you happen to have one of the genetic variants that can push it up.
In fact the questions of whether or not measuring CRP would improve coronary risk prediction is the subject of three papers and two editorials in the July 10, 2006 issue of the Archives of Internal Medicine and the July 4, 2006 issue of the Annals of Internal Medicine. In the July 10, 2006 issue of the Archives of Internal Medicine, a team led by Dr Aaron R. Folsom from the University of Minnesota in Minneapolis reported the results of the Atherosclerosis Risk in Communities (ARIC) study, which assessed the association of 19 novel risk markers with incident CHD in 15 792 adults followed up since 1987-1989.
The participants underwent a physical examination, including assessment of major risk factors, at the beginning of the study and every three years afterward. At four times during the follow-up period, researchers collected blood and DNA samples for analysis. Patients continue to be tracked for the development of CHD. Novel markers included measures of inflammation, endothelial function, fibrin formation, fibrinolysis, B vitamins, and antibodies to infectious agents.
Folsom concluded that:
“C-reactive protein level does not emerge as a clinically useful addition to basic risk-factor assessment for identifying patients at risk of a first CHD event. Routine screening is not warranted for any of the other 18 novel risk factors tested, either.”
Another study from Brigham and Women’s Hospital in Boston did suggest that CRP might be helpful in predicting coronary disease in some women. But in an editorial, George Davey Smith from the University of Bristol in England had this to say:
“There are many reasons for skepticism about the role of CRP as a predictor of CHD: CRP may not be causally related to CHD; it remains more expensive than asking patients about their health, lifestyle, and socioeconomic background; and it adds only modest additional predictive ability over conventional risk factors, even in Cook and colleagues’ (i.e. the Brigham and Women’s) study.”
The moral of the story? Random measurements of CRP have not been shown to be of much value.
And be a bit cautious about medical advice on Fox News.
Deep Vein Thrombosis
I am sorry to hear that the United States Vice-President Dick Cheney has just developed a blood clot in his leg and is being treated with anticoagulants (blood-thinning medications) that he will need to be on for several months.
He experienced some discomfort in his lower left leg this morning, and the diagnosis of deep vein thrombosis was made.
Mr Cheney is now 66 years old and has a history of cardiac problems. He has suffered at least four myocardial infarctions (heart attacks) and has a pacemaker.
He had quadruple bypass surgery in 1988 after his third heart attack.He also had an operation to remove blood clots around his knees in 2005.
Mr Cheney recently returned to Washington after long flights to Japan, Australia, Pakistan and Afghanistan.
As I discussed a few months ago deep vein thrombosis – often shortened to "DVT" – can be associated with long-distance flying because it leads to inactivity and dehydration. Not, as was formerly thought, low oxygen pressure.
Blood clots in the legs are not in themselves life-threatening but they can be dangerous if they become wedged in the lungs (pulmonary embolism) or other organs, which can in severe cases be fatal.
Although the venous and arterial sides of the circulation are often thought of as quite different, it is not that unusual for someone to have problems in both, either because of immobility, metabolic disturbances or low grade inflammation.
With Spring Break and early summer vacations coming up, please don’t forget to keep moving when you are on planes, limit the alcohol and coffee cnsumption, and have plenty of water to drink.
Bon voyage!
Air Pollution and Cardiovascular Disease

There a very important piece of research published in this week’s issue of the prestigious New England Journal of Medicine, indicating that air pollution increases the risk of cardiovascular disease, at least in women. The whole article is available for free download.
Researchers from the University of Washington studied 65,893 postmenopausal women without previous cardiovascular disease in 36 U.S. metropolitan areas from 1994 to 1998, with a median follow-up of 6 years. All the participants were aged 50 to 79 and part of the Women’s Health Initiative, a major US Government funded investigation into the causes of heart disease in women. A total of 1,816 women suffered one or more cardiovascular event.
The investigators were particularly interested in tiny airborne particles called particulates, which are less than 2.5 microns across, and can lodge in the lungs. Previous research had incriminated them in heart disease. These are the dense clouds that you see coming out of chimneys or exhaust pipes. They found that pollution levels varied between four to nearly 20 micrograms per cubic meter.
Each 10 microgram rise was matched by a 76% rise in the chances of dying from heart disease or stroke. For women living within, rather than between, cities, the risk more than doubled, increasing by 128%, with each step up in pollution levels.
It is not clear whether women are more susceptible to pollution than men. Women’s coronary arteries are smaller and this might render them more vulnerable.
These results suggest that the risk from air pollution is far greater than most doctors previously thought, though it is still not clear how these sooty particles lead to the development of heart disease.
I live just outside a city where we often have smog advisories for weeks at a time in the summer. This research adds to the growing evidence that air pollution should be taken seriously as a risk factor for cardiovascular disease.
That also means that when localized air pollution is particularly high, people with chronic lung disease or coronary heart disease should avoid staying outside.
This problem will likely get worse as the summers be progressively warmer.
Yet another reason for taking climate change seriously.
“For the first time in the history of the world, every human being is now subjected to contact with dangerous chemicals, from the moment of conception until death.”
–Rachel Carson (American Biologist and Writer, 1907-1964)
Tea and Milk

Growing up in England, tea is a great deal more than a drink.
Always drunk hot, of course. No normal person would want it served cold.
It is a major social lubricant and is considered by most to be a separate food group. And the health benefits conferred by a nice cup of tea are now known to just about everyone in Britain.
But from an early age I knew that one day I would have to leave the country.
Why?
Because I could never abide the way in which the vast majority of tea drunk in England is destroyed by the addition of milk and sugar. There are even long technical debates about whether to add the milk before pouring in the tea or after? How fast to add the white stuff? How to stir it in?
Since I was knee high to a puppy I was always the odd one out, wanting nothing to do with this wanton destruction of a sublime beverage.
Which should always be enjoyed au naturel. The only thing that might ever sully a cup of fine Earl Grey or Darjeeling might be a little lemon. Anything else?
Yuk.
Well, it now transpires that this isn’t just a matter of taste buds.
A study just published in the European Heart Journal says it all in the title, “Addition of milk prevents vascular protective effects of tea.”
Tests on sixteen healthy postmenopausal female volunteers showed that black tea significantly improved the ability of the arteries to relax and expand, but adding milk completely blunts the effect. The research was supplemented by tests on rat blood vessels. Tea caused the muscle in the vessel wall to relax by producing nitric oxide from the endothelial cells that line blood vessels. Adding milk blocked the production of nitric oxide and the relaxation of the muscles.
Now bear in mind that they were testing black tea. The researchers are now looking at the potentially more potent green tea to see whether its effects are also blocked by milk.
The villain of the piece is a group of proteins called caseins, which they found interacted with the tea to decrease the concentration of catechins in the beverage. Catechins are the flavonoids in tea that mainly contribute to its protection against cardiovascular disease.
The moral of the story? Tea can be wonderful on so many levels. Not only does it taste good, but also it can do wonders for your health.
But please, please, please don’t lose all the benefits by sloshing in a load of milk!
Raw, naked tea is the way to go…
“Thank God for tea! What would the world do without tea? How did it exist? I am glad I was not born before tea.”
–Sydney Smith (English Clergyman and Essayist, 1771-1845)







