Acupuncture for Hay Fever
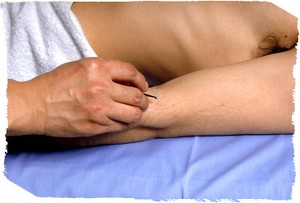
A study from Melbourne, Australia has found that acupuncture can significantly reduce the symptoms of persistent allergic rhinitis (PAR), a.k.a. hay fever. This was a randomized, single-blind, sham-controlled trial included 80 patients with PAR aged 16-70 years, who were randomly assigned to real or sham acupuncture. Three key acupuncture points, Yingxiang L.I.-20, Yintang M-HN-3 and Fengchi GB-20, plus one supplementary point (determined individually on the basis of traditional Chinese Medicine pattern differentiation) were used for each participant. After a one-week baseline period, participants were treated twice weekly for eight weeks and followed up for another 12 weeks. Nasal obstruction, sneezing, rhinorrhea and nasal itch were each self-assessed daily on a 5-point scale, and individual symptom scores were added to give a sum of the symptom scores: total nasal symptom score (TNSS). A secondary outcome was use of PAR relief medication. At the end of eight weeks’ treatment, the weekly mean difference in TNSS from baseline was significantly greater with real (-17.2) than with sham acupuncture (-4.2) and these benefits persisted three months after the end of treatment. Comparisons of relief medication scores revealed a significant decline in the use of medication in the real acupuncture group between baseline and Week 8 of treatment, the reduction being still apparent at the end of follow-up.
This research is convincing. The effect size is not enormous, and we do not know how long the effect will last, but it does suggest another approach for people who have chronic symptoms and for whom medications are ineffective, or who do not want to take medications, or have side effects from them.
It may be relevant that some years ago it was shown that needling the Fengchi point – which lies at the base of the skull at the back of the head – increases some components of cerebral blood flow. That may give us a mechanism of action of the acupuncture in this trial.
“I am pretty sure that, if you will be quite honest, you will admit that a good rousing sneeze, one that tears open your collar and throws your hair into your eyes, is really one of life’s sensational pleasures.”
–Robert Charles Benchley (American Humorist, Critic and Parodist, 1889-1945)
“The nose is for breathing, the mouth is for eating.”
–English Proverb
“Warmth, moisture, food-these are the causes that activate latent germs and arouse them to activity. They exist, all except the food, in the mouth, nose and throat at all times. The food is thrown out into these, as excretions, in disease. The germs feed on the excretions. They are scavengers. They were never anything else and will never be anything else. They break up and consume the discharge from the tissues. This is the function ascribed to germs everywhere in nature outside the body and is their real and only function in disease. They are purifying and beneficial agents. The medical profession has worked itself into hysteria over the germ theory and is using it to exploit an all too credulous public. Germs are ubiquitous. They are in the air we breathe, the food we eat, the water we drink. We cannot escape them. We can destroy them only to a limited extent. It is folly to attempt to escape disease by attempting to destroy or escape germs. Once they are in the body, the physician has no means of destroying them that will not, at the same time, destroy the patient. We cannot avoid germs. We must be proof against them. We have to accept them as one of the joys of life.”
–Herbert Shelton (English Evolutionary Philosopher, 1820-1903)
Non-pharmacological and Lifestyle Approaches to Attention-Deficit/Hyperactivity Disorder: 1. Diet

You can find some articles on Attention-Deficit/Hyperactivity Disorder (ADHD) here, and also some of the evidence that ADHD is a “real” illness and not just a label for socially unacceptable behavior. That being said, it is essential to take extra care when making the diagnosis. Mud sticks, and diagnostic mud sticks like glue. It can be hard to “unmake” a diagnosis.
As with any problem, the most effective way of helping it is to address the physical, psychological, social, subtle and spiritual aspects of the situation.
Medicines can definitely have a place in the management of ADHD, and the reason for treating ADHD is not so that people get better grades in school or do better at their jobs. It is to prevent the long term problems that may follow from inadequately treated ADHD.
There is a large and growing body of research on non-pharmacological approaches to treating ADHD. A literature search has turned up over two hundred papers, over half of which report some empirical research. Some of the research is summarized in a short paper aimed at health care professionals.
Research has shown that more than 50% of American families who receive care for ADHD in specialty clinics also use complementary or alternative medical (CAM) therapies, if you include things like modifying their diet or other aspects of their lifestyle. Despite that, only about 12% of families report their use of CAM to their clinician. Despite that low rate of families reporting the use of unorthodox therapies, a national survey of pediatricians showed that 92% of them had been asked by parents about complementary therapies for ADHD. The trouble is that many pediatricians have not been taught very much about the pros and cons of these approaches.
The most commonly used CAM therapies for ADHD are dietary changes (76%) and dietary supplements (> 59%). I have talked about food additives and one type of diet in the past. Now let’s look in a little more detail.
The 3 main dietary therapies for ADHD are:
- The Feingold diet,
- Sugar restriction, and
- Avoiding suspected allergens.
Sometimes these diets are used in combination.
The Feingold Diet
The Feingold diet is the most well known dietary intervention for ADHD. It aims to eliminate 3 groups of synthetic food additives and 1 class of synthetic sweeteners:
Synthetic colors (petroleum-based certified FD&C and D&C colors);
Synthetic flavors;
BHA, BHT and TBHQ ; and
The artificial sweeteners Aspartame, Neotame, and Alitame.
Some artificial colorings such as titanium dioxide are allowed.
During the initial weeks of the Feingold program, foods containing salicylates (such as apples, almonds, and grapes) are removed and are later reintroduced one at a time so that the child can be tested for tolerance. Most of the problematic salicylate-rich foods are common temperate-zone fruits, as well as a few vegetables, spices, and one tree nut.
During phase 1 of the Feingold diet, foods like pears, cashews, and bananas are used instead of salicylate-containing fruits. These foods are slowly reintroduced into the diet as tolerated by the child.
The effectiveness of this diet is controversial. In an open trial from Australia, 40 out of 55 children with ADHD had significant improvements in behavior after a 6-week trial of the Feingold. 26 of the children – 47.3% – remained improved following liberalization of the diet over a period of 3-6 months.
In another study, 19 out of 26 of children responded favorably to an elimination diet. What is particularly interesting is that when the children were gradually put back on to a regular diet, all 19 of them reacted to many foods, dyes, and/or preservatives.
In yet another study, this one a double-blind, placebo-controlled food challenge in 16 children, there was a significant improvement on placebo days compared with days on which children were given possible problem foods. Children with allergies had better responses than children who had no allergies.
Despite this research many pediatricians, particularly in the United States, do not believe the evidence regarding the effectiveness of elimination diets or additive-free diets warrants this challenging therapy for most children.
There is an interesting difference in Europe. In 2004 a large randomized, blinded, cross-over trial of over 1800 three-year-old children was published. The results showed consistent, significant improvements in the children’s hyperactive behavior when they were on a diet free of benzoate-preservatives and artificial flavors. They had worsening behavior during the weeks when these items were reintroduced. On the basis of this and other studies, in 2004 schools in Wales banned foods containing additives from school lunches. It has been claimed that since the ban, there has been an improvement in the afternoon behavior of students.
The biggest problem with the Feingold and other elimination diets is that they are hard to follow and to maintain. But for some children and families, the inconvenience and stricter attention to food have worthwhile results.
It is also essential to ensure that children on any kind of diet maintain adequate nutrition: there have been many examples of that simple rule not being followed.
Sugar Restriction
The notion that sugar can make children “hyper” entered the mainstream over twenty years ago, and is now on the list of things that “everyone knows.” But happily it is not true. At least 12 double-blind studies have failed to show that sugar causes hyperactive behavior. Some researchers suggest that sugar or ingestion of high-carbohydrate “comfort foods” is actually calming, and that children who seek these foods may be attempting to “self-medicate.”
There are plenty of very good reasons for children to avoid candy, but hyperactivity is not one of them.
Food Allergies
There is clear evidence that children, and perhaps adults with ADHD are more likely to have allergies. That lead to the obvious question whether children with ADHD allergic or sensitive to certain foods. (It is useful to differentiate “allergies” that are the result of abnormal reactivity of the immune system to proteins in food, from “sensitivities” that are the direct result of substances in food: the two have different treatments.)
It is certainly true that food allergies and food sensitivities can generate a wide range of biological and behavioral effects. Gluten sensitivity (celiac disease) is known to be linked to an increased risk of ADHD and other symptoms.
In an open study of 78 children with ADHD referred to a nutrition clinic, 59 improved on a few foods trial that eliminated foods to which children are commonly sensitive. For the 19 children in this study who were able to participate in a double-blind cross-over trial of the suspected food, there was a significant effect for the provoking foods to worsen ratings of behavior and to impair psychological test performance.
For more than 30 years one of the tests used to track allergies has been the radioallergosorbent test (RAST). It is not much used these days since technology has moved on. In an allergy testing study of 43 food extracts 52% of 90 children with ADHD had an allergy to one or more of the foods tested. Over the next few years several researchers carried out open-label studies in which children with ADHD and food allergies were treated with a medicine called sodium cromoglycate, that prevents the release of inflammatory chemicals such as histamine from mast cells. Some of the reports suggested that it could help in some children.
Other popular dietary interventions include eating a low glycemic index diet to avoid large swings in blood sugar. Another strategy has been to “go organic” to reduce the burden of pesticides, hormones, antibiotics, and synthetic chemicals in the child’s system. These diets need more scientific study but they are probably safe if expensive.
There are plenty of practitioners and commercial entities who claim to be able to identify food sensitivities with all kinds of methods from blood and muscle testing to electrical and energetic techniques. Some may be helpful, but few have been proven to be effective.
What Should Parents do About Diet, Nutrition, Allergies and Sensitivities?
It is very difficult to predict whether an individual child will be helped by changes in diet. However, as long as the child’s needs for essential nutrients are met these diets should be safe.
It is an extremely good idea for parents to keep a diet diary for one to two weeks to see if anything obvious jumps out. Then trying an additive-free diet, low in sugar and avoiding foods that are suspected of exacerbating symptoms. You will normally find the answer – yes or no – within a few weeks.
What is the Evidence for Food Sensitivities and ADHD in Adults?
Not a lot!
There are plenty of people who have reported that dietary restrictions have helped them, but there is very little evidence. One of the problems about looking for food sensitivities is that there is a high placebo response rate. But if you have adult ADHD, it may be worth investigating. Just make sure that any diet that you use is nutritionally sound. And if you don’t find anything reconsider another approach.
Asthma, Air and Allergies

After a couple of weeks away I was distressed to see that I was going to be returning to a city which has just been rated as the most challenging place in America for people with asthma.
This is the list according to the Asthma and Allergy Foundation of America:
- Atlanta
- Philadelphia
- Raleigh, North Carolina
- Knoxville, Tennessee
- Harrisburg, Pennsylvania
- Grand Rapids, Michigan
- Milwaukee
- Greensboro, North Carolina
- Scranton, Pennsylvania
- Little Rock, Arkansas
I am pleased to say that I do not have asthma, though I have a strong family history of it. If you live in one of these cities, or any other with a high rate of pollution, there is nothing much to be done apart from:
Staying indoors when the weather is bad
Using an air purifier
Keep to a diet designed to reduce your risk of inflammation
Use homeopathy and tapping therapies to help when necessary.
And sadly, for some people, medicines are the only option. But I always try the other approaches as well.
Self-hypnosis and Hay Fever
I first learned to do hypnosis in 1980, and I have always found it a useful adjunctive treatment for some people, though in recent years I have spent far more tie teaching people to use self-hypnosis.
The research data on hypnosis has also been growing, to the extent that nearly two years ago an article in the Mayo Clinic Proceedings, a fairly conservative journal, suggested that the time had come for an expanded role for hypnosis in general medicine as well as a study of different techniques that are in use.
Hypnosis and self-hypnosis may affect an illness directly, or it might reduce a trigger to the illness, say if anxiety triggers an asthma attack, we could use hypnotherapy to treat the anxiety. Hypnosis may improve a person’s subjective responses to the illness. It might also be useful to help counteract side effects in people who just have to be treated with conventional medications.
Many case reports of apparent cures with hypnosis have found their way into the popular press. I have mentioned that over a period of five years I spent one to two days a week going through and checking most of these reports in all the languages that I can read. Sadly some of them turned out not to hold much water.
But now the quality of the research has improved enormously. I have been particularly impressed with some of the studies on allergy: it is very remrakable to think that we can make specific suggestions that produce demonstrable effects on the immune system. I particularly liked a study from Switzerland that was published in the journal Psychotherapy and Psychosomatics.
A team from Basel University taught 66 people with hay fever how to do self-hypnosis and found that it helped them to alleviate symptoms such as runny nose.
The volunteers also took their regular hay fever medicines, but the effect of hypnosis appeared to be additive so that they could reduce the doses that they needed to take.
The study took place over two years and included two hay fever seasons. During the first year, one group of the volunteers with hay fever were taught and asked to regularly practice hypnosis as well as take their usual allergy medicine. The training consisted of one two-hour session with an experienced trainer. The remaining volunteers had no other treatment apart from their normal allergy medication.
After a year, the researchers found the volunteers who had been using self-hypnosis had reported fewer symptoms related to hay-fever than their fellow volunteers.
During the second year, the researchers taught the remaining "untrained" volunteers how to use hypnosis. By the end of this year, these volunteers also reported improvement in their hay-fever symptoms.
Although the improvement in symptoms was not statistically significant the researchers also found that the volunteers had cut down on the amount of hay fever medication they used after learning self-hypnosis.
There is another interesting piece of research on this topic. You will probably have experienced a histamine reaction: the typical wheal, flare and swelling that can occur after, say, an insect bite. Researchers form Denmark used hypnosis to induce emotions of sadness, anger, and happiness, to see whether these emotions would have any effect on the skin’s response to histamine. Not only did mood have an effect on the skin reactions, but also people who were more susceptible to hypnosis were more reactive to histamine.
Hypnosis is being used with many clinical conditions, from asthma to migraine and irritable bowel syndrome. It is not a panacea, but it can be a very useful tool. And it tells us a lot about the power of the mind to influence virtually every system of the body.
Food Additives and Behavior

Few things generate as much heat and as little light as the debate about a possible association between food additives and cognition, mood and behavior.
There are a number of ways in which food may influence all three, including:
- Malnutrition
- Composition of the diet
- Nutrient quality of the diet
- Eating habits
- Pharmacological effects of foods
- Food allergy
- Food sensitivity
- Contamination of food with heavy metals, hormones and pesticides
- Fatty acid deficiency
- Food additives
It is often surprising to learn that many people do not realize that in children – particularly if malnourished – omitting breakfast can have a marked effect on cognitive functioning. But it is the last of those that I want to look at today.
Until the 1950s if food manufacturers wanted to add color to a food it was done primarily with natural plant and vegetable based compounds: pale red colors could be achieved from beets; green from chlorophyll-containing vegetables; yellows and orange could be achieved from extracts from a number of other plants and spices. But then things began rapidly to change as we outlined in Healing, Meaning and Purpose.
The notion that food additives could be a cause of hyperactivity is at least 30 years old. I think that Ben Feingold was the first to introduce the idea and with it his notoriously difficult diet.
Over the years there have been some positive clinical trials of the diet and some negative. But I think that every clinician working with behavior problems has seen some startling improvements in some children and adolescents when they go on an elimination diet.
In 1985 a controversial study published in the Lancet claimed to show that 79% of hyperactive children had symptomatic improvement when food chemicals were removed from their diet. Then when the food chemicals were re-introduced the symptoms returned. No other study has ever produced figures anything like that high.
It is also important that in young children, though additives may cause a problem in some, there does not seem to be a link between allergies and food sensitivities, and parents often pick up behavior changes that simple clinical screening tools do not. So mom and dad may really know best.
Several years ago we tried to look at the impact of food additive not on behavior, but on headache. When the additives were administered double blind, we were unable to replicate most people’s symptoms, even when they were sure that a certain food caused a problem.
However, unsupervised restriction diets are not without their dangers. And we also need to make sure that practitioners know what they are doing: I once saw a young woman who had seen by an “alternative allergist,” who had left her on a diet consisting of spring water, rice and lettuce. And nothing else.
Another problem is that many of us do not know what additives are lurking in the food that we eat. There was a recent study in the United Kingdom indicated that on average, Britons consume 20 different food additives every day, with some eating up to 50. Yet most people were unaware of this figure, with nearly half of the 1,006 people surveyed thinking they ate only 10 additives each day.
The research also found that many people did not understand which foods are most likely to contain additives. I have not yet seen the raw data from this study, but I shall have more to say about it once it becomes available.
A number of large independent studies are currently underway (for example, here) which should help us to better identify who is susceptible to additives, how to test for sensitivity to additives and who might benefit from their withdrawal.
The trouble with a lot of the discussion about food additives, behavior, mood and cognition is that it usually begins from a false premise: that there is a single cause for a behavior.
When I am teaching it continues to astonish me that most health care professionals still expect there to be one “cause” for a problem. Yet as I have mentioned before, this is rarely clinical reality.
A food additive may be associated with problems, but only in a minority of children, and only if they are genetically predisposed and if the right set of environmental circumstances are in place.
If you suspect a problem, first, learn to look at labels. And see if simple exclusion helps. An allergist is the next stop, but also ask whether an additive could be causing a biochemical rather than an allergic problem. If it is a biochemical effect, it may not show up on routine allergy tests, but there are other ways of testing.
The Red Tide

There is an important report about the impact of environmental change in this month’s issue of the journal Chest.
Red tide is a common name for a phenomenon known as an algal bloom,
a well known event in which marine algae accumulate rapidly in the
water column, or “bloom”. These algae, more correctly termed phytoplankton, are microscopic, single-celled, plant-like organisms that can form dense, visible patches near the water’s surface. We know that red tides have been occuring in the Gulf of Mexico for centuries, but they appear to be spreading and to be becoming more common and severe.
The main type of plankton is a species of dinoflagellate known as Karenia brevis, that is concentrated along shorelines and produce highly potent aerosolized toxins. The new research shows that Florida red tide toxins – called brevetoxins can impact respiratory function and increase respiratory symptoms in patients with asthma.
In otherwise healthy people inhaled aerosolized red tide toxins can lead to eye irritation, runny nose, postnasal drip, nonproductive cough, and wheezing. The symptoms usually subside after leaving beach areas. But things can be far more serious for people with asthma, who may experience respiratory problems and decreased lung function after just one hour of beach exposure to the toxins.
This was a fine piece of research funded by the National Institute of Environmental Health Sciences, and makes it clear that not only that asthma sufferers need to be aware of this potential source of trouble but that we all need to be alert to the possibility that human activities are increasing the red tide and with it, the risk of further health problems.
Stress and the Skin
You have probably noticed how stress can have an impact on some people’s skin. Increasing stress can initiate or worsen skin disorders such as psoriasis and atopic dermatitis. There has also been a lot of discussion about whether stress can also exacerbate acne and cause cold sores to erupt.
A new study published in the December issue of the American Journal of Physiology-Regulatory, Integrative and Comparative Physiology sheds important light on this association.
It is well known that one of the physical effects of stress is to increase levels of a range of steroid hormones called glucocorticoids. The best known glucocorticoid is cortisol or hydrocortisone. So the question was whether the missing link between stress and skin problems might be one or other of the glucocorticoids.
Researchers from the Veterans Affairs Medical Center, San Francisco and the University of California at San Francisco and Yonsei University Wonju College of Medicine, Wonju, Korea decided to study this possible connection.
You may have heard that the skin is the largest organ in the body and provides the critical barrier between the environment and the internal organs. Its most important function is providing a permeability barrier that prevents us from drying out. When we are healthy we are approximately 65-70 percent water. We are able to survive and function in dry environments because the skin forms a permeability barrier that prevents the loss of water.
The physical location of the permeability barrier is in the outermost layer of the epidermis that is known as the stratum corneum. The stratum corneum is composed of dead cells surrounded by lipid membranes. The stratum corneum layer continuously sloughs off, and therefore has to be constantly regenerated. The epidermal cells in the lower epidermis are continuously proliferating to provide new cells, which then differentiate, move toward the surface and ultimately die, to form a new the stratum corneum. This process is going on in your skin right now, though it can be disrupted by damage such as sunburn. If the process becomes overactive, it can lead to the development of thick, hardened skin.
It was already known that psychological stress disturbs this elegantly balanced system by decreasing the proliferation of epidermal cells and inhibiting their differentiation. As a result the function of the permeability barrier is impaired.
To test the hypothesis that glucocorticoids would have adverse effects on skin function, they stressed some hairless mice by putting them in small cages in constant light and forcing them to listen to the radio for 48 hours.
Before being stressed one group of mice was treated with mifepristone, which you may know by its two other names, RU-486, or the “morning after” pill, which blocks the action of glucocorticoids. A second group was given a drug called antalarmin, which blocks glucocorticoid production. A third group was stressed but received neither drug and a fourth group remained unstressed in ordinary cages and without the continuous light and sound to which the other groups were exposed.
The mice that received mifepristone or antalarmin showed significantly better skin function compared to the stressed mice that did not receive either treatment.
The experiment demonstrated the important role that glucocorticoids play in inducing the skin abnormalities brought on by psychological stress. Although we hope that the study will lead to a way to treat people who suffer from these skin conditions, there is still a long way to go. It’s always difficult to extrapolate from mice to people. Second, there may be serious side effects of modulating glucocorticoid activity. Glucocorticoids are essential hormones that play many important roles. Blocking their action could have negative outcomes. This is one of the reasons why we are skeptical about advertisements that claim that some herbal concoction can “cure” cortisol-related obesity. If something could really modify the activity of cortisol or other glucocorticoids in the body, it would likely have many most undesirable effects.
The research team is now looking at the effect of psychological stress on the skin’s production of antimicrobial peptides, which play a role in defense against infection. It has long been thought that psychological stress might also reduce the ability of the skin to protect from infections.
I never like to leave a report involving animal experiments without also saying a heartfelt thank you to the animals that participated in the experiments.
This research is interesting and may have a number of spin offs. But I have another rather obvious question: since we already know that there is a link between stress and some skin problems, why not focus on stress management techniques, rather than trying to find new medicines to help counteract the biochemical effects of stress?
Update on Pramipexole
I have mentioned pramipexole before. In the United States it is approved for the treatment of the signs and symptoms of idiopathic Parkinson’s disease.
I’m always on the look out for medicines that can be part of a package of healthcare, and we need to learn both the pros and cons of new medicines. This looks to be a medicine that can be incorporated into Integrated Medicine. And before you ask, I have no links at all with the manufacturer, Boehringer Ingelheim.
There have been a number of interesting papers presented at the 10th International Congress of Parkinson’s Disease and Movement Disorders in Kyoto, Japan this week.
New data presented have shown that people taking pramipexole (Mirapexin®/ Sifrol®) can experience significant improvements in a broad range of symptoms associated with Restless Legs Syndrome (RLS).
In all studies presented at the meeting, people taking pramipexole reported clinically meaningful improvements in both their night and day-time symptoms, as measured on the International Restless Legs Scale (IRLS). The IRLS measures several aspects of the condition, ranging from discomfort, the need to move around, relief by moving around and then more specific RLS symptoms such as sleep disturbance, day-time tiredness, mood disorder, as well as addressing overall severity, weekly frequency, daily severity, and impact on daily activities.
One of the big problems in the treatment of RLS is that people who have it frequently have other problems as well, such as hypertension, arthritis, gastroesophageal reflux disease, depression, anxiety, and diabetes. So it is essential that the physical component of treatment should not cause any deterioration in associated illnesses. One of the papers presented in Kyoto indicated that pramipexole could be used in people with RLS who are also taking an array of other medicines. That claim is going to have to be checked by the FDA, but the data look very encouraging.
Still, when using medications, there’s no such thing as a free lunch: The most commonly reported adverse reactions in clinical trials for RLS were nausea, headache, and tiredness.
In people with Parkinson’s disease, pramipexole may cause them to fall asleep without any warning, even while doing normal daily activities such as driving. This is obviously very serious, and before the medicine gets an RLS indication in the USA, the FDA will really check this out in great detail. When taking pramipexole hallucinations have been known to occur and sometimes patients may feel dizzy, sweaty or nauseated upon standing up. In Parkinson’s disease, there is also a warning that as with many other medicines used to treat it, including pramipexole may be associated with impulse control disorders/compulsive behaviors.
So we need to keep an eye on safety, but so far the data is very encouraging, and we may soon have something else to add to an integrated treatment program for people with RLS.
___________
Here’s a P.S. On November 10th, 2006, pramipexole was approved for use in RLS by the FDA. Here’s the announcement:
Ingelheim/Germany, 10 November 2006 – Boehringer Ingelheim announced today that the U.S. Food and Drug Administration (FDA) has approved pramipexole, a non-ergot dopamine agonist, for the treatment of moderate to severe primary Restless Legs Syndrome (RLS).1 This is an important milestone for pramipexole (Mirapexin® / Sifrol® / Mirapex®), which was already approved throughout the European Union in April 2006 for this second indication.
Women, Asthma and the Brain
There’s been a longstanding puzzle in medicine. Well actually there are lots of them, but here’s one that may be a puzzle no more.
For many years now, it’s been known that asthma is more common in women, and also that psychological stress can cause flare ups of asthma.
Many women experience “menstrual flaring:” a worsening of asthma around the time of their menstrual period. There is also a strange paradox: some women with asthma wheeze less if they take an oral contraceptive, while some non-asthmatic women begin to wheeze when they take it. In some women pregnancy makes asthma worse, and in others it affords months of relief of symptoms. Women who are obese are more likely to get asthma, presumably because their intra-abdominal fat stores are churning out inflammatory mediators.
Researchers from the University of Wisconsin have shed some important light on this link between asthma and the brain. In research published in the Proceedings of the National Academy of Sciences. In the study, six patients with mild asthma were exposed to ragweed or dust-mite extracts. The subjects were shown three different categories of words: asthma-related (e.g., "wheeze"), non-asthma negative ("loneliness") or neutral ("curtains").
Using functional magnetic resonance imaging, they showed that activity in two regions, known as the anterior cingulate cortex and the insula showed increased activity when the asthma-related words were heard compared with the other types. What is more, this enhanced activity was specifically linked to physiologic signals from the ragweed and dust-mite extracts. So being exposed to asthma-relevant emotional stimuli is associated with markers of inflammation and airway obstruction in asthmatic people exposed to an asthma-producing antigen.
In people with asthma and other stress-related conditions, these brain regions may be hyper-responsive to disease-specific emotional and physiologic signals. Taken together, these could contribute to problems that worsen the asthma, such as inflammation.
And one of the ways of making these regions of the brain hyper-responsive? Bathe them in estrogen.
That still does not explain why pregnancy and the oral contraceptive makes some women’s asthma better, and does the opposite in others. But it may just have to do with the “set point” of the cells in these regions of the brain. In the same way that we might set the thermostat in out house. An already hyper-responsive brain might be normalized and an under-active one stimulated to be over-active.
We need to do some more experiments, but these are a great start.
If you ever wheeze, have a look to see if there are stressors or hormonal events that trigger you. Whether you are being treated with homeopathy, herbals or conventional therapy, knowing when to expect trouble gives you the power to adapt you treatment when you are entering a risky time in your life.






