The Causes and Consequences of Insulin Resistance
I have spent so much time talking about insulin resistance becuase it is one of the greatest medical threats facing the world.
It is estimated that approximately 33% of the adult population of the United States is insulin resistant, and if left untreated many will develop diabetes, hypertension and an array of other problems. It is an epidemic that is expected to swamp most health care systems around the world, yet sadly it may in most cases be preventable.
There is an enormous literature on insulin resistance. As of this afternoon there are almost 33,000 scientific papers on the subject.
I created this graphic to try and summarize the key points about insulin resistance: the main factors that may cause it, as well as the most important medical consequences.
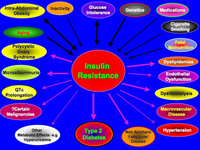
(Click on the graphic to expand it.)
The Main Causes of Insulin Resistance are:
- Aging
- Intra-abdominal obesity
- Inactivity
- Glucose intolerance
- Genetics
- Fetal malnutrition
- Cigarette smoking
- Some medications
The Main Consequences of Insulin Resistance are:
- Type 2 diabetes mellitus
- Hypertension
- Arteriosclerosis
- Polycystic ovarian syndrome
- Non alcoholic fatty liver disease
- Disturbances in the function of the vascular endothelium
- Elevations of triglycerides and cholesterol
- Disturbances of clotting
- Disturnaces in kidney function
- DIsturbances in one type of heart rhythm
- Elevated uric acide levels
- Some malignancies
This is probably not a complete list, but it gives you a very good idea of the reasons for looking for insulin resistance. Many – but not all – experts now recommend measuring insulin resistance in people at high risk of developing any of these medical problems.
We have good evidence that lifestyle changes can prevent the development of many of these dire consequences, so it is certainly something worth discussing with your health care provider.
Insulin Resistance, Diabetes and the Timing of Meals
At a meeting of the American Diabetes Association in June 2006, Professor Markus Stoffel from the Eidgenossische Technishe Hochschule in Zurich and Rockefeller University in New York, received the Outstanding Scientific Achievement Award for his extremely interesting and important research on the molecular mechanisms involved in the developmental insulin resistance.
This may sound as interesting as watching paint dry, but in actual fact the research is supremely practical, and may lead to a complete re-working of some commonly used dietary strategies.
Many physicians have not yet been taught that the liver is the key organ involved in the genesis of insulin resistance and of type 2 diabetes mellitus. Up to 90% of the glucose circulating in your blood has come from your liver. As the liver becomes less sensitive to the actions of insulin, it starts producing more glucose, particularly after meals. This in turn causes blood glucose to rise and with it insulin levels. One of the other consequences of insulin resistance is that the liver stops storing triglycerides, which then start circulating, while at the same time storing other types of fat, leading to what we call, not surprisingly, fatty liver. Or in the dog Latin that doctors use to confuse the general public, hepatic steatosis.
When we are fasting, the liver switches on banks of genes that produce the enzymes responsible for oxidizing fatty acids to produce fuel.
The main objective of a balanced diet is to maintain balance: we want to avoid sudden swings in glucose, fatty acids or insulin: it is these sudden changes that can cause inflammatory changes in blood vessels and in the liver and may lead to some of the circulatory problems that are such distressing complications of diabetes. We want to try and keep our insulin levels smooth and low. The best way not to do that is to have frequent high calorie snacks and to eat late at night. The best way is to follow the plans that I’ve talked about before. Eat little and often, keep the balance of nutrients just right, and be aware of the exact times at which you eat. Nothing except a little protein in the 2-3 hours before you retire for the night, and go very easy on alcohol, which can wreck your metabolism.
“The secret of life is balance, and the absence of balance is life’s destruction.”
–Hazrat Inayat Khan (Founder of the Sufi Order of the West, 1882-1927)
Technorati tags: Insulin resistance Diabetes mellitus Fasting Weight management
How Many Angels Can Dance on the Head of a Needle? Moving Beyond the Metabolic Syndrome
I have written a great deal both on this blog and in scholarly articles, about insulin resistance and the insulin resistance and metabolic syndromes.
You will have noticed that I’ve always used the term insulin resistance syndrome.
This is not a matter of semantics. For years now I’ve been worried about the splitting that’s been going on in the field: we currently have six sets of definitions of the metabolic syndrome. And apart from the fun of going to all those conferences in exotic parts of the world, you have to ask what’s been achieved by these ever more divisive attempts to “define” the medical consequences of insulin resistance.
The American Diabetes Association has begun to promote the concept of “cardiometabolic risk.” The Association has established a national Cardiometabolic Risk Initiative (CMRI) to stress the association between diabetes, heart disease and stroke. The idea of introducing this umbrella term is to help people better understand and manage all diabetes and cardiovascular risk factors, and to side-step some of the controversy surrounding the definition of insulin resistance or metabolic syndrome and which cluster of variables are in and out.
A new Cardiometabolic Risk (CMR) Calculator to help us evaluate an individual’s risk of diabetes or vascular disease should be available by the end of the year.
The formula already includes factors such as:
1. Body mass index
2. Waist circumference ratio
3. Fasting plasma glucose
4. HDL-cholesterol
5. LDL-cholesterol
6. Triglycerides
7. Apolipoprotein B
8. Blood pressure
9. C-reactive protein
10. Age
11. Sex
12. Race/ethnic origin
13. Family history
14. Tobacco use
Part of the reason for this new initiative is the discovery that pre-diabetes, or impaired fasting glucose, where plasma glucose levels are 100-125 mg/dl, is associated with a high prevalence of cardiovascular disease risk factors such as obesity, hypertension and dyslipidemias.
The person who first proposed the insulin resistance syndrome, a.k.a. syndrome X, a.k.a. metabolic syndrome, is Gerald Reaven who first recognized the syndrome in a landmark paper in 1988. He recently gave a lecture entitled; “Insulin Resistance Versus Metabolic Syndrome: Different Names, Different Concepts, Different Goals.” I am in complete agreement with his basic proposition, which is that insulin resistance explains the clustering of all of the components that make up the metabolic syndrome. So Gerry’s position is that there’s no point in trying to make a diagnosis of metabolic syndrome: everything is due to insulin resistance.
So instead of wasting time and resources in trying to diagnose metabolic syndrome, it is much better to understand the pathophysiology: what is going on at the molecular level, how these processes produce risk factors, and whether we can predict others. We should identify and treat each of the underlying processes and the complications of insulin resistance. If we are going to have a syndrome, it should be called insulin resistance syndrome.
And let’s stop these academic debates and get on with the job at hand: there is a 600% variation in peoples’ ability to have insulin transport glucose into cells. More than half the US population is destined to develop at least some degree of insulin resistance, so we need to look for better ways to identify people who have it, and to apply the principles of integrated medicine to keeping them healthy.
Technorati tags: Insulin resistance Insulin resistance syndrome Metabolic syndrome Cardiovascular disease Hypertension Inflammation Hyperlipidemia Weight gain Integrated medicine






