Spicy Foods as Cancer Killers

Several news services have picked up a very important piece of research in the February 16th issue of the journal Biochemical and Biophysical Research Communications.
In a nutshell, they have shown that capsaicin, an ingredient of jalapeno peppers, triggers cancer cell death by attacking mitochondria, the energy producing organelles in the cell. Some of the reports were a little confused and confusing and also missed out some critical pieces.
So first, a bit of revision, this is a graphical representation of what a mitochondrion looks like:
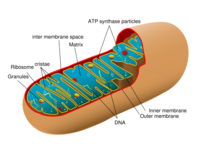
The mitochondrion is the primary producer of energy in the cell, converting molecules derived from food or stores into adenosine triphosphate (ATP) and several other less important molecules. ATP is the energy “currency” throughout the body. In recent years we have discovered that there are a number of diseases that are a result of faulty mitochondrial metabolism.
One of the biggest problems about most forms of chemotherapy for cancer is that the treatments often damage normal cells as well as the malignant ones. Therefore a great deal of research has aimed at identifying differences between normal and malignant cells.
Over the last ten years, increasing evidence has shown that mitochondrial dysfunction is a key feature of many types of cancer as well as part of normal aging. This has lead to the idea that we might have a new therapeutic target if cancer cell mitochondria are different from those in normal cells.
This new study showed that the family of molecules to which capsaicin belongs, the vanilloids, bind to proteins in the cancer cell mitochondria to trigger apoptosis – programmed cell death – without harming surrounding healthy cells. Capsaicin was tested on cultures of human lung and pancreatic cancer cells.
As the lead researcher Timothy Bates has said, “We believe that we have in effect discovered a fundamental ‘Achilles heel‘ for all cancers.”
This is extraordinarily interesting, not least because capsaicin is already in use for the topical treatment of peripheral neuropathy and some inflammatory conditions of the skin including psoriasis. The amount of capsaicin used in the experiments was similar to amounts that could probably be ingested safely. So now the next step if to see whether these observations can be translated into a viable treatment option for cancer, and if so, which types.
What the research does not say is that eating a lot of spicy food will help prevent or treat cancer.
The reports that I have seen have failed to mention that one of the reasons for doing this research was that some spices have been used in traditional Chinese and Indian medicine for many centuries for the treatment of several conditions, and some of the investigators are engaged in the Nottingham UK–China Collaboration on Complementary and Alternative Medicine.
How many more treasures are waiting for us in the archives of traditional medicine?
And how many have already been lost as plant and animal species become extinct?
The Price of False Weight Loss Claims
It has just been reported that this afternoon the United States Federal Trade Commission has recovered more than $25 million ro settle allegations of deceptive marketing for four products:
- Xenadrine EFX
- CortiSlim
- TrimSpa
- One-A-Day WeightSmart
This is not a surprise. For anyone with any knowledge of human metabolism some of the claims made in television and print advertisements were really far-fetched.
The fines may sound large, but are probably just a drop in the bucket for the companies.
This legal action is all about false claims, but there is another worry, and that is that some of the alleged weight-loss products may also have side effects. Two months ago I mentioned that there are currently investigations underway of at least two people who appeared to have developed manic symptoms while on Cortislim. It remains to be seen if there is a causal relationship.
Pretty much ANYTHING will help you lose weight in the short term. But if these products really worked and were safe, then why on earth wouldn’t doctors and nurses be using them themselves and prescribing them to their patients?
Sad to say weight loss does not come in a bottle: I only wish that it did!
Stick with the principles of gradually modifying your diet, exercise and be aware of the psychological traps that can sabotage healthy living. And please don’t waste your money on quick fixes that cannot possibly work.
If it seems too good to be true, then it probably is.
Attention Deficit Disorder and Omega-3 Fatty Acids
Six months ago we discussed some of the research linking allergy, disturbances of cell membranes and attention deficit disorder with or without hyperactivity (ADD/ADHD). I also drew attention to the work indicating that there might be a role for omega-3 fatty acids in treatment, the essential fatty acid found primarily in seafood and flaxseed oil. The link between omega-3 fatty acids and ADD/ADHD has come from five lines of evidence:
- If animals are deprived of this nutrient, they become hyperactive and their offspring have reduced cognitive abilities
- Omega-3 fatty acids are essential to the normal growth of the brain
- Studies in animals indicate that changing the dietary intake of omega-3 fatty acids impacts the all-important dopamine systems of the brain
- Children who are breast fed have lower rates of ADD/ADHD, which is independent of any maternal characteristics ,and breast milk contains many essential nutrients including omega-3 fatty acids
- Anecdotes and some clinical trials of omega-3 fatty acids in children with ADD/ADHD, though we still don’t know the best way to supplement
Well, the research continues to come thick and fast:
- Omega-3 fatty acid deficiency may be involved in aggression, hyperactivity and conduct disorder, though the evidence is not as strong as it is for some other nutrients: Iron, zinc and protein deficiency all seem to contribute to aggressive, hyperactive behavior.
- Another recent study has found low levels of omega-3 fatty acids in children with ADHD.
- There seems to be an association between ADHD and a deficiecny of a key enzyme in fatty acid metabolism called fatty acid desaturase 1.
All of this led to the announcemet on Friday that the Murdoch Childrens Research Institute in Melbourne, Australia is recruiting for a clinical trial of the effects of omega-3 fatty acids on the brain function of children with ADHD. The study will examine the effects of these fatty acids on the learning skills, attention span, memory, reaction time and behaviour of 150 children with ADHD over 12 weeks. The effects will also be explored in 100 children without ADHD.
I am encouraged by the way in which the investigators plan to do this work, and I shall keep you posted as data – whether positive or negative – continues to emerge from this study and others.
An Aspirin a Day Keeps the Prostate Away?
Well I promise that that is going to be my only cheesy title his week. But I couldn’t resist after seeing some interesting new research published in this month’s issue of American Journal of Epidemiology.
As they age, many men develop an enlargement of the prostate gland, technically known as benign prostatic hyperplasia, can make urination difficult or trigger a need to urinate frequently. This can be particularly troublesome if men keep having to get up at night to pass urine.
The researchers decided to look at the potential impact of non-steroidal anti-inflammatory agents (NSAIDs), because they had previously been shown to reduce the risk of prostate cancer. The study was well designed and involved 2,447 men in a single county in Minnesota. Taking NSAIDs was found to significantly prevent or delay enlargement of the prostate.
We must be cautious: we don’t want to encourage men to take NSAIDs inappropriately: they can have many side effects, and more work is needed to confirm the findings, and then to find the optimum dose to cut risk.
This is useful information. I’m not keen on taking any medicine on a long-term basis; particularly not a class of medicines that can cause gastrointestinal upset and increase the risk of bleeding. But this research follows hard on the heels of one large negative study on the widely used herbal remedy Saw Palmetto.
This is a brief extract from something that I wrote for another program:
Saw Palmetto (Serenoa Repens) is also known as Sabal, American dwarf palm tree and Cabbage palm. As its name implies, it is a member of the palm family.

Uses and Indications:
It is primarily used in the management of prostate enlargement. Some early studies suggested that Saw Palmetto reduces the symptoms of benign prostatic hypertrophy through antagonism of both androgens and estrogens.
It only increases urine flow and does not decrease the size of the prostate. In a review of 18 randomized trials involving approximately 3,000 men, Saw Palmetto did provide overall benefit on prostatic symptoms. However, it is not certain how long any effect might last. In a one year prospective study, comparing Saw Palmetto with finasteride, (Proscar), the herb had no appreciable benefit, whilst the finasteride did. There was however no placebo arm in the study, and no measures of the patients’ subjective well-being.
If the herb is going to help it usually takes 4-6 weeks or longer for effects to be observed.
More recently, some women have been exposed to Saw Palmetto, since it sometimes an ingredient of those herbal concoctions that are supposed to increase bust size.
Cautions and Side Effects:
Saw Palmetto is a cause of gynecomastia in men. It may also have gastrointestinal side effects of nausea and diarrhea.
Saw Palmetto may cause insomnia, fatigue and headaches.
Due to its anti-androgenic and anti-estrogenic effects Saw Palmetto is contraindicated in:
Pregnancy (or in women at risk of becoming pregnant)
Breastfeeding
Hormonal dependent illnesses (e.g., prostate or breast cancers)
Drug interactions:
Oral contraceptives and any hormone replacement therapy such as conjugated estrogens.
Saw Palmetto contains tannins, and these may interfere with the absorption of iron.
If given with warfarin, there is an increased chance of bleeding.
Decaffeinated Coffee

Your humble reporter has always been skeptical about all those people who ask for decaf coffee because it is supposed to be somehow safer and not cause insomnia.
Not only have I had the philosophical question, “How can chemically altering a natural substance be safer?!” but I’ve seen plenty of people with all the clinical signs of caffeinism after only drinking decaffeinated coffee. You probably know – or perhaps have experienced – the key features:
- Restlessness
- Nervousness
- Excitement
- Insomnia
- Flushed face
- Diuresis (passing excessive amounts of urine)
- Gastrointestinal disturbance
- Muscle twitching
- Rambling flow of thought and speech
- Tachycardia or cardiac arrhythmia (Fast heart rate or irregularity of the heart)
- Periods of inexhaustibility
- Psychomotor agitation
People vary greatly in their sensitivity to caffeine. It is also important to know that caffeine can interact with some medications like lithium and anxiolytics.
Now researchers from the University of Florida College of Medicine in Gainesville, Florida and ConeChem Research in Maryland have published an interesting paper in the Journal of Analytical Toxicology.
The researchers tested ten cup of decaf coffee collected from nine independent and national coffee establishments. They found that drinking five or more mugs of coffee could have the same kick as drinking one or two cups of regular coffee.
The conclusion: you need to know that decaffeinated coffee can contain significant amounts of caffeine that may cause you all kinds of symptoms, as well as possible interfering with the actions of some herbal and homeopathic remedies.
“Moderately drunk, coffee removes vapours from the brain, occasioned by fumes of wine, or other strong liquors; eases pains in the head, prevents sour belchings, and provokes appetite.”
–England’s Happiness Improved (1699)
Multiple Sclerosis and Integrated Medicine
Although there are some fairly effective conventional therapies for multiple sclerosis (MS), many people with MS explore complementary and alternative medicine (CAM) therapies for their symptoms. The most effective strategies are to combine conventional and unorthodox treatments that address the physical, psychological, social, subtle and spiritual aspects of the illness. This combined approach also avoids the problem of people taking herbs or supplements that may either interact with each other or with conventional treatments.
It is also essential for us to get over the idea that MS is just something to be conquered. That may seem like an odd comment, but the language and the mindset of fighting, battles and warfare can be problematic. Let me explain something that I discuss at length in Healing, Meaning and Purpose.
There have been two distinct approaches to health in the Western medical tradition. The first is that the role of a physician is to treat diseases. That is the way that all my colleagues and I were trained. The second approach is to consider that health is the natural order of things. So in the first case we constantly hear the use of military metaphors: People speak of “a war on cancer,” “killer cells,” “magic bullets,” and the need to adopt a “fighting spirit.” Sadly this aggressive attitude by the medical profession may be at odds with the wishes and needs of an individual, the family and the other people in a person’s life. We have to try to strike a balance between the whole instinct to fight and expressions of healing and acceptance.
In the second case, the philosophy is grounded in the idea that we need to work in harmony with nature. The maintenance of health and well being comes from reestablishing balance and harmony not just in ourselves but also in our relationships with each other, with society and with the entire environment around us.
Some of the most commonly CAM therapies include dietary modification, nutritional and herbal supplementation, and mind-body therapies. There has been a revival of interest among MS researchers about the therapeutic potential of low-fat diet and essential fatty acid supplementation in MS. The research on CAM therapies in MS is still exploratory, but considering peoples’ interest and common use of these therapies, further research in this area is clearly warranted. Many sufferers show “spontaneous” recoveries, so reports of cures with unorthodox remedies are often treated with skepticism.
Diet, Vitamins and Supplements: There have been scattered reports of symptoms improving after the removal of dental amalgam, but there is scant evidence that this is really worthwhile. There is some evidence 1. 2. 3. 4. that polyunsaturated fatty acid (PUFA) supplementation may help MS. There used to be a lot of support for something called the “Swank diet,” but over the years the evidence has not been very good. In a small number of people with MS certain foods can make them worse. This is to expected if there is an autoimmune component to the illness. It is always a good idea to see if there is something that makes a person feel worse. The other important qestion is whether food additives may be causing symptoms. Although this must be uncommon, I have written elsewhere about occasional cases of MS symptoms with all the classical neurological, biochemical, radiological and electrical signs that have improved or become completely better after removing aspartame from the diet.
Physical exercise: Exercise is highly recommended for people with MS, though it is best to avoid it during an attack. There is evidence that over-exertion can actually bring on an attack. There is some literature about the use of Feldenkrais bodywork in MS, but a study from the University of North Carolina failed to find any benefit. T’ai Chi Ch’uan, qigong, yoga and graduated exercise have all been helpful to some people with MS, but it is essential to discuss it with a healthcare provider to see how any one of these fits in to an package of care. There is no published data on the use of Pilates in MS. At least not in any of the languages that I can read. But since it has been shown to improve posture and flexibility, it is logical to think that Pilates might be helpful, and it would be very valuable to see some research on it.
Acupuncture: Although widely used, the research on acupuncture in MS is not yet convincing. Like most acupuncturists I’ve had some good results in treating pain, muscle stiffness and fatigue. I’ve also seen people achieve some remarkable recoveries, but there are two issues: MS is a relapsing and remitting illness. And second, many of the people who did well only did so because they shifted their thinking: acupuncture became the vehicle for their personal transformation rather than a device for removing nasty symptoms.
Homeopathic remedies: Even the most enthusiastic homeopaths have fairly limited expectations of what homeopathy can achieve in MS.
From the point of view of homeopathy there is little point in making the diagnosis on multiple sclerosis because the disease has such a variable course with highly variable symptoms. To a homeopath the diagnosis is not useful: it is the symptoms that are all important. The homeopathic treatment of MS is highly individualized: one of the key items is the timing of symptoms and associated features. Some of the most common remedies for people with MS are:
- Agaricus
- Alumina
- Argentum Nitricum
- Arsenicum
- Aurum Metallicum
- Causticum
- Cocculus
- Conium Maculatum
- Ignatia
- Lachesis
- Nux Vomica
- Natrum Muriaticum
- Phosphorus
- Plumbum
This is not the whole list of homeopathic remedies that we have sometimes found helpful, but it highlights some of the more commonly used ones in people with the symptoms of MS.
Herbal remedies: Many herbal remedies have been tried in MS, and many experts have told me that they have had some good results. There is an important issue in MS called “apitherapy,” a.k.a. bee venom therapy (BVT). Several reports suggest that bee venom may be an effective treatment for patients with MS. But formal trials suggest that although the treatment appears relatively safe apart from itching and swelling of the skin, it does not seem to be helpful.
The best approach is to embrace the best of what conventional medicine has to offer, combine unorthodox approaches and to realize that management of a chronic illness is not about dominating it but learning from it and learning strategies for peacefully co-existing with it.
À Votre Santé!

I am a wine buff. Several years ago I did a one year training with the Wine and Spirit Education Trust which turned me from a dilettante to someone who knew how to understand the subtlety of wines from one end of a vineyard or another. Oh yes, and how to get very good wine for not many $$.
I also learned a whole range of other new skills. Ever since then I’ve been interested in the health consequences of drinking wine. Of course, too much of a good thing isn’t. But there has been so much evidence that certain types of wine, when used in moderation, can do wonderful things for your health.
This week has seen the publications of a paper in the journal Nature, that has been described by Steve Bloom from the Imperial College Faculty of Medicine like this: “It could be the breakthrough of the year, with massive possibilities for treating human beings.”
Steve is not given to hyerbole, so what has got him so passionate?
The answer is that a chemical found in dark grapes and in red wine called resveratrol, that could make guilt-free gluttony a reality.
Why is this?
Previous research has revealed the substance has anti-ageing effects in some organisms, extending the lifespan of yeast by 60%, worms and flies by 30%, and fish by about 60%.
It has also been suggested the reported health benefits of red wine may also be due to resveratrol.
When given to mice, it countered some effects of a high-calorie diet, with 60% of the calories coming from fat, improving their health and increasing their life-span. The mice showed decreased glucose levels, healthier hearts and liver tissue, and better motor function compared with the mice on the same diet but without the supplement.The chemical could not reverse all consequences of overeating – the mice did not lose any weight.
The researchers also discovered that the chemical was extending the mice’s life-span. The scientists estimated resveratrol reduced the risk of death in the mice by about 31%. After six months, resveratrol essentially prevented most of the negative effects of the high calorie diet in mice.
The exact mechanism of the chemical is not yet known, but the researchers believe it may be activating a gene called SIRT1, which is linked to a family of proteins thought to be involved with longevity.
This is not yet an invitation to enjoy limitless quatities of grapes or wine: a glass of red wine has only 0.3% of the relative resveratrol dose given to the gluttonous mice.
BTW, you may be interested to know that Nature is now providing an excellent podcast based on papers in this week’s edition.
Turmeric and Arthritis
I recently reported about some research from SIngapore that indicated that the spice turmeric might help with cognition.
Today there is a study form the University of Arizona in the journal Arthritis and Rheumatism suggesting that the spice may also be helpful in experimental rheumatoid arthritis. In line with most other studies of herbal supplements it is interesting that the maximal effect was obtained by using the natural form of turmeric, that contains three major "curcuminoids," the likely active ingredients. If one of the three is missing, the effect is a lot less.
The extracts appears to work by preventing the activation of a protein that controls when genes are switched on or off in the joint. Once the protein known as NF-KB is activated, it binds to genes and increases the production of inflammatory proteins, which in turn attack the joints.
This is not a surprise: In traditional Indian Ayurvedic medicine turmeric has been used for centuries as a treatment for inflammatory disorders including arthritis. Based on that, dietary supplements containing turmeric rhizome and turmeric extracts have been sold for years. However, there’s been little direct evidence that they are helpful.
We are going to need more research before we can sy whether turmeric supplements can be recommended for medicinal pruposes, and eating more spices is unlikely to work.
These findings are opening up a new approach to treating not just rheumatoid arthritis, but perhaps also other inflammatory diseases such as inflammatory bowel disease, asthma and multiple sclerosis. Interestingly the turmeric extract also has another effect: it deactivates a biochemical pathway that leads to the resorption of bone. So it may help with osteoporosis.